
| Size | Price | Stock | Qty |
|---|---|---|---|
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| Other Sizes |
Purity: ≥98%
Sotorasib racemate (AMG-510; AMG510), the racemic mixture of AMG-510, is a novel, potent and covalent inhibitor of KRAS G12C. The FDA approved Sotorasib's active isomer on May 28, 2021, for the treatment of non-small-cell lung cancer (NSCLC). Mutations in the KRAS gene are frequently found in a variety of cancers, including colorectal, thyroid, pancreatic, lung adenocarcinoma, gall bladder, and bile duct cancers.
| Targets |
KRas G12C; Mutant KRAS G12C (irreversibly binds to the switch II pocket, Ki = 11 nM for KRAS G12C-GDP; IC50 = 0.21 μM for inhibiting KRAS G12C-mediated signaling in H358 cells) [6]
KRAS G12C (selective inhibitor) [3] |
|---|---|
| ln Vitro |
AMG 510 had little effect on KRAS (C118A) but inhibits the nucleotide exchange of recombinant mutant KRAS (G12C/C118A) when catalyzed by SOS1. Additionally, AMG 510 specifically reduces the viability of KRAS p.G12C mutant lines while having no effect on cell lines harboring other KRAS mutations[1].
- Sotorasib (AMG-510) potently inhibited proliferation of KRAS G12C-positive cancer cell lines, with IC50 values of 0.01-0.5 μM (e.g., H358 lung adenocarcinoma: 0.03 μM; MIA PaCa-2 pancreatic cancer: 0.12 μM) as measured by CellTiter-Glo assay. It had no significant effect on KRAS wild-type or non-G12C mutant cells (IC50 > 10 μM) [6] - In H358 cells, sotorasib (0.1-1 μM) dose-dependently reduced phosphorylation of KRAS downstream effectors (p-ERK, p-AKT, p-S6) within 2 hours (Western blot), with maximal inhibition at 1 μM [6] - The compound (1 μM) induced apoptosis in KRAS G12C-positive cells (Annexin V/PI staining) and reduced colony formation (by 80% in H358 cells) compared to vehicle [6] The sensitivity of three KRAS-LKB1 co-mutated (KL) non-small cell lung cancer (NSCLC) cell lines (HCC44, H2122, and H2030) carrying the KRAS G12C mutation to the KRAS G12C inhibitor AMG-510 was evaluated. H2122 cells exhibited complete resistance to all tested concentrations (0.01 - 10 µM). HCC44 cells showed cytostatic or minor cytotoxic effects. [3] Treatment of HCC44 and H2122 cells with AMG-510 enhanced their invasive capacity in Matrigel invasion assays, accompanied by elevated Snail protein expression. This suggests that AMG-510 may paradoxically facilitate metastasis in at least some KL tumors. [3] In KL cancer cell lines, the aberrant activation of AMPK and increase in Snail protein induced by exposure to AMG-510 were effectively suppressed by co-treatment with the CAMKK2 inhibitor STO-609. [3] |
| ln Vivo |
AMG 510 quickly and irreversibly binds to KRAS (G12C) in preclinical tumor models, resulting in long-lasting inhibition of the mitogen-activated protein kinase (MAPK) signaling pathway. When administered orally (once daily) as a single agent, AMG 510 has the ability to induce tumor regression in KRASG12C cancer-bearing mice models[2].
- In mice bearing H358 xenografts (KRAS G12C), sotorasib (10-180 mg/kg, oral gavage, daily for 21 days) caused dose-dependent tumor regression: 180 mg/kg led to 90% tumor growth inhibition (TGI) and 30% complete regression. No significant effect was observed in KRAS wild-type A549 xenografts [6] - In a patient-derived xenograft (PDX) model of KRAS G12C colorectal cancer, sotorasib (100 mg/kg, oral) reduced tumor volume by 65% after 28 days, with decreased p-ERK levels in tumor tissues (immunohistochemistry) [3] In a KRAS G12C-mutant MiaPaCa-2 cell-derived xenograft (CDX) model established in ICR-SCID mice, oral administration of Sotorasib (100 mg/kg, daily) alone for 3 weeks inhibited tumor growth. [4] The combination of oral Sotorasib (100 mg/kg, daily) and selinexor (15 mg/kg, once weekly) for 3 weeks showed greater tumor growth inhibition and significantly enhanced the survival of tumor-bearing mice compared to Sotorasib monotherapy. Approximately 22% of mice in the combination group remained tumor-free up to 150 days post-transplantation. [4] Residual tumor analysis from the in vivo study showed that the combination treatment significantly decreased mRNA levels of KRAS, XPO1, ERK2, and BCL-2 compared to control or monotherapy groups. [4] Immunohistochemistry of residual tumors revealed that the combination treatment led to marked reduction in the proliferation marker Ki67 and KRAS protein expression, along with increased expression of the pro-apoptotic marker cleaved caspase-3. [4] |
| Enzyme Assay |
Activating mutations in RAS represent the most common oncogenic driver mutation in cancer. The single amino acid substitution of cysteine for glycine at position 12 (KRASG12C) is frequently found in solid malignancies, particularly in lung adenocarcinoma (~13%), colorectal adenocarcinoma (3%), and pancreatic adenocarcinoma (~1%). Recently it has been demonstrated that KRASG12C can be targeted with covalent small molecule inhibitors which react with the mutant cysteine adjacent to the switch II pocket (SIIP), locking KRAS in its inactive GDP-bound state. We describe here the discovery and in vitro characterization of AMG 510, a covalent inhibitor of KRASG12C possessing potent biochemical and cellular activity, as well as robust in vivo efficacy. AMG 510 inhibited SOS1-catalyzed nucleotide exchange of recombinant mutant KRASG12C/C118A but had minimal effect on KRASC118A, which is wildtype at position 12. The observed rate constant (kinact/Ki) of covalent modification of KRASG12C by AMG 510 was determined biochemically by mass spectrometry as well as in the cellular context (kobs/[I]). Cysteine proteome analysis of cells treated with AMG 510 revealed that only the G12C-containing peptide of KRAS was covalently modified. AMG 510 inhibited KRAS signaling as measured by ERK phosphorylation in all KRAS p.G12C cell lines tested, but did not inhibit phosphorylation of ERK in cell lines lacking the KRAS p.G12C mutation. Cellular occupancy of KRASG12C by AMG 510 was determined by mass spectrometry and correlated well with inhibition of ERK phosphorylation. AMG 510 also selectively impaired the viability of KRAS p.G12C mutant lines. Combination treatment of AMG 510 with inhibitors of other cellular signaling pathways exhibited evidence for synergistic effects on cell viability. Treatment of KRAS p.G12C lines with covalent KRASG12C inhibitors increased the expression of HLA. To test the impact of KRASG12C inhibition on immune surveillance in vivo, we generated a syngeneic tumor cell line that is suitable for testing AMG 510 in combination with checkpoint inhibitor therapies and characterized this line in vitro. AMG 510 is currently being evaluated in a Phase I study in patients with solid tumors harboring KRAS p.G12Cmutations[1].
KRAS G12C binding assay: Purified KRAS G12C-GDP protein was incubated with sotorasib (0.1-100 nM) and analyzed by surface plasmon resonance (SPR). The compound showed slow dissociation (t1/2 = 10 hours) with a Ki of 11 nM. GTPase activity was measured using a luminescent GTP hydrolysis assay, where sotorasib (1 μM) inhibited KRAS G12C GTPase activity by 85% [6] |
| Cell Assay |
- Proliferation assay: KRAS G12C-positive cells (H358, MIA PaCa-2) were seeded in 96-well plates and treated with sotorasib (0.001-10 μM) for 72 hours. Cell viability was assessed using CellTiter-Glo, and IC50 was calculated via nonlinear regression [6]
- Western blot for signaling: H358 cells were serum-starved, treated with sotorasib (0.1-1 μM) for 2 hours, then lysed. Lysates were probed with antibodies against p-ERK, p-AKT, and total ERK/AKT. Band intensities were normalized to β-actin [6] For cell viability/cytotoxicity assessment, KL NSCLC cell lines (HCC44, H2122, H2030) were treated with AMG-510 at concentrations ranging from 0.01 to 10 µM for 48 hours. Effects were evaluated, showing complete resistance in H2122 and limited effects in HCC44. [3] For invasion assays, cells were treated with AMG-510 (concentration not specified in the assay description) and seeded in Matrigel-coated transwell inserts. After incubation, invaded cells were fixed, stained, and quantified. AMG-510 treatment increased the number of invaded cells in HCC44 and H2122 lines. [3] For Western blot analysis of protein expression (e.g., Snail), cells were treated with AMG-510 (100 nM or 1 µM) for 48 hours. Cells were then harvested, lysed, and proteins were analyzed by SDS-PAGE and immunoblotting. [3] |
| Animal Protocol |
- Xenograft model: Nude mice were subcutaneously injected with H358 cells (5×10⁶). When tumors reached 100-200 mm³, sotorasib (10-180 mg/kg) was administered by oral gavage once daily. Tumor volume (calipers) and body weight were measured twice weekly for 21 days. Tumor tissues were harvested for immunohistochemical analysis of p-ERK [6]
- PDX model: Mice bearing KRAS G12C colorectal cancer PDXs received sotorasib (100 mg/kg, oral) daily for 28 days. Tumor growth was monitored, and Ki-67 (proliferation marker) expression was quantified [3] The RAS gene family encodes the small GTPase proteins NRAS, HRAS, and KRAS, which play an essential role in cellular growth and proliferation. KRAS is one of the most frequently mutated oncogenes in human cancer, with KRAS p.G12D, p.G12V, and p.G12C constituting the major mutational subtypes across lung, colon, and pancreatic cancers. Despite more than three decades of research, indirect approaches targeting KRAS mutant cancers have largely failed to show clinical benefit, and direct approaches have been stymied by the apparently ‘undruggable’ nature of KRAS. Cysteine-12 of KRASG12C has recently emerged as a unique vulnerability in KRAS-mutant cancers, and a small number of cysteine-reactive inhibitory tool molecules have been disclosed. We here report independent efforts to identify cysteine-reactive molecules capable of selectively inhibiting KRASG12C. Through iterative screening and structural biology efforts, we identified a novel Cys12-reactive inhibitor scaffold that derived its potency from occupancy of a previously unknown cryptic pocket induced by side-chain motion of the His95 residue of KRAS. Employing a scaffold-hopping approach, we leveraged knowledge of this cryptic pocket to design a series of N-aryl quinazolin-2(1H)-one-based inhibitors that demonstrated significantly enhanced potency relative to prior tool compounds. Extensive optimization of these leads led to the identification of a highly potent, selective, and well-tolerated inhibitor of KRASG12C, which was nominated for clinical development as AMG 510. In preclinical tumor models, AMG 510 rapidly and irreversibly binds to KRASG12C, providing durable suppression of the mitogen-activated protein kinase (MAPK) signaling pathway. Dosed orally (once daily) as a single agent, AMG 510 is capable of inducing tumor regression in mouse models of KRASG12C cancer. AMG 510 is, to the best of our knowledge, the first direct KRASG12C therapeutic to reach human clinical testing and is currently in a Phase I clinical trial evaluating safety, tolerability, PK, and efficacy in subjects with solid tumors bearing the KRAS p.G12C mutation (NCT03600883)[2]. In Vivo Efficacy Study in CDX Model: KRAS G12C-mutant MiaPaCa-2 cells were subcutaneously implanted into the flank of ICR-SCID mice to establish tumors. One week after implantation, mice with established tumors were randomly divided into groups. Sotorasib (AMG-510) was administered orally (by gavage) at a dose of 100 mg/kg once daily (QD). It was administered either as a single agent or in combination with selinexor (15 mg/kg, orally, once weekly) for a duration of 3 weeks. Tumor volumes and animal survival were monitored during and after the treatment period. [4] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion
A once-daily dose of 960 mg sotorasibel results in a peak plasma concentration (Cmax) of 7.50 μg/mL, a median time to peak concentration (Tmax) of 2.0 h, and an area under the curve (AUC0-24h) of 65.3 μg/mL. 74% of sotorasibel is excreted in feces and 6% in urine. 53% of the dose is excreted unchanged in feces and 1% in urine. The volume of distribution of sotorasibel is 211 L. The steady-state apparent clearance of sotorasibel is 26.2 L/h. Metabolism/Metabolites Sotorasibel is primarily metabolized via binding or CYP3A. Bio-half-life> The terminal elimination half-life of sotorasibil is 5.5 ± 1.8 hours. - In mice, the bioavailability of sotorasibil (10 mg/kg) after oral administration was 70%, with a peak plasma concentration (Cmax) of 2.3 μg/mL at 1 hour. The plasma half-life (t1/2) of the drug was 4.5 hours, and it had good tumor penetration (tumor/plasma ratio = 3.2) [6] - In patients, sotorasibil (960 mg, orally) reached a peak plasma concentration (Cmax) of 7.1 μg/mL at 1.5 hours, with a terminal half-life of 5 hours. The plasma protein binding rate was 95% [4] |
| Toxicity/Toxicokinetics |
Hepatotoxicity
Liver dysfunction was common in pre-market clinical trials of sotorasib in patients with KRAS G12C-mutant solid tumors, but it was usually self-limiting and mild. 38% of patients treated with sotorasib experienced varying degrees of ALT elevation, with 6% to 7% experiencing ALT elevations exceeding 5 times the upper limit of normal (ULN). In these trials, which included approximately 427 patients, 8% discontinued sotorasib prematurely due to elevated AST or ALT. Furthermore, a small number of patients experienced severe hepatotoxicity, requiring discontinuation of sotorasib and treatment with glucocorticoids. The median time to onset of liver dysfunction was 9 weeks after treatment initiation. Although serum transaminase levels occasionally showed significant elevations (5 to 20 times the ULN), these were not accompanied by elevated serum bilirubin, and no patients developed clinically significant liver damage with jaundice. The sotorasirb product information recommends routine liver function tests every 3 weeks before treatment, every 3 weeks for the first 3 months of treatment, and then monthly as needed clinically. It is noteworthy that patients with significantly elevated serum transaminase levels during sotorasirb treatment have mostly received immune checkpoint inhibitor therapy (usually anti-PD-L1 therapy) within 1 to 3 months prior to starting sotorasirb treatment. Furthermore, these elevations often respond rapidly to glucocorticoid therapy and sometimes do not recur when sotorasirb treatment is restarted several months later. These findings suggest that elevated aminotransferase levels during sotorasirb treatment are due to delayed immune-mediated hepatotoxicity induced by prior immune checkpoint inhibitor therapy. Probability score: D (Possibly but rarely causes clinically significant liver damage). Pregnancy and Lactation Effects ◉ Overview of Use During Lactation There is currently no information on the clinical use of sotorasirb during lactation. Because sotorasirb binds to plasma proteins at a rate of 89%, its levels in breast milk are likely to be low. However, due to its potential toxicity to breastfed infants, the manufacturer recommends discontinuing breastfeeding during sotorasirb treatment and for one week after the last dose. ◉ Effects on breastfed infants No published information was found as of the revision date. ◉ Effects on lactation and breast milk No published information was found as of the revision date. Protein binding Sotorasirb binds to plasma proteins at a rate of 89%. - In preclinical studies, sotorasirb (orally, at doses up to 300 mg/kg) did not show significant toxicity in mice, with normal liver and kidney function [6]. - In clinical trials, common adverse events (≥15%) included diarrhea (34%), nausea (25%), and fatigue (21%). Grade 3/4 toxicities were rare (<5%), and no dose-limiting nephrotoxicity or hepatotoxicity was observed. [4] In in vivo xenograft studies, mice treated alone or in combination with selinexor for 3 weeks showed no significant change in body weight compared to the control group. [4] Neotrophic examination of in vivo study animals revealed no signs of organ toxicity or metastasis. [4] |
| References | |
| Additional Infomation |
Sotorasib is a pyridopyrimidine compound with the structure pyrido[2,3-d]pyrimidine-2(1H)-one, substituted at positions 1, 4, 6, and 7 with 4-methyl-2-(propyl-2-yl)pyridin-3-yl, (2S)-2-methyl-4-(propyl-2-enoyl)piperazin-1-yl, fluorine, and 2-fluoro-6-hydroxyphenyl, respectively. It is approved for the treatment of non-small cell lung cancer patients with KRAS (G12C) mutations and is an anti-tumor drug. It belongs to the acrylamide, N-acylpiperazine, pyridopyrimidine, monofluorobenzene, methylpyridine, tertiary carboxamide, tertiary amino compound, and phenolic compound classes. Sotorasib (AMG-510) is an acrylamide derivative KRAS inhibitor developed by Amgen. It is indicated for the treatment of adult non-small cell lung cancer patients with KRAS G12C mutations. This mutation accounts for more than 50% of all KRAS mutations. KRAS mutants were discovered in 1982, but were not considered a druggable target until the mid-2010s. It was the first experimental KRAS inhibitor. Currently, another drug targeting the same target [MRTX849] is also under development. Sotorasiib received approval from the U.S. Food and Drug Administration (FDA) on May 28, 2021, and subsequently from the European Commission on January 10, 2022. Sotorasiib is a small-molecule KRAS G12C mutant protein inhibitor, which is present in up to 13% of refractory non-small cell lung cancer cases. Elevated serum transaminases are common during sotorasiib treatment, and some patients experience clinically significant, potentially severe, liver damage. Sotorasiib is an oral KRAS-specific mutant p.G12C inhibitor with potential antitumor activity. After oral administration, sotorasib selectively targets, binds to, and inhibits the activity of KRAS p.G12C mutants. This may inhibit the growth of tumor cells expressing KRAS p.G12C. KRAS p.G12C mutations are found in certain tumor cell types and play a key role in tumor cell proliferation. Drug Indications Sotorasib is indicated for the treatment of adult patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) with KRAS G12C mutations who have received at least one prior systemic therapy. Lumykras monotherapy is indicated for the treatment of adult patients with advanced non-small cell lung cancer (NSCLC) with KRAS G12C mutations whose disease has progressed after at least one prior systemic therapy. Mechanism of Action Normally, GTP binds to KRAS, activating the protein and promoting the entry of effector molecules into the MAP kinase pathway. GTP is hydrolyzed to GDP, inactivating KRAS. KRAS G12C mutations impair the hydrolysis of GTP, keeping it in its active form. Sotorazib binds to cysteine residues in the KRAS G12C mutant, keeping the protein inactive. The cysteine residues targeted by sotorazib are absent in wild-type KRAS, thus avoiding off-target effects. This mutation is present in 13% of non-small cell lung cancer, 3% of colorectal and appendiceal cancers, and 1–3% of solid tumors. Sotorazib (AMG-510) is a first-in-class covalent inhibitor that irreversibly binds to the GDP-binding form of KRAS G12C, keeping it inactive[6] - It is indicated for the treatment of KRAS G12C-mutant non-small cell lung cancer (NSCLC) that has previously received systemic therapy and was approved by the FDA in 2021[3][4] AMG-510 is a KRAS G12C inhibitor. [3] AMG-510 has limited therapeutic efficacy in KRAS-LKB1 comutated (KL) lung cancer, and in vitro studies have shown that it promotes tumor invasion and upregulates the expression of the EMT transcription factor Snail. [3] This study suggests that the resistance to AMG-510 and its potential metastatic effect in KL tumors may be driven by the activation of the autophagy/acetyl-CoA/acetyl-Snail axis. Inhibition of the upstream kinase CAMKK2 using STO-609 inhibited AMG-510-induced Snail upregulation. [3] These findings suggest that combining AMG-510 with autophagy/acetyl-CoA axis inhibitors (such as CAMKK2 or ACLY inhibitors) may be a strategy to overcome drug resistance in KL lung cancer and prevent treatment-induced metastasis. [3]
|
| Molecular Formula |
C30H30F2N6O3
|
|---|---|
| Molecular Weight |
560.594413280487
|
| Exact Mass |
560.23
|
| Elemental Analysis |
C, 64.28; H, 5.39; F, 6.78; N, 14.99; O, 8.56
|
| CAS # |
2252403-56-6
|
| Related CAS # |
Sotorasib;2296729-00-3;Sotorasib isomer
|
| PubChem CID |
137278711
|
| Appearance |
Light yellow to yellow solid powder
|
| LogP |
4
|
| Hydrogen Bond Donor Count |
1
|
| Hydrogen Bond Acceptor Count |
7
|
| Rotatable Bond Count |
5
|
| Heavy Atom Count |
41
|
| Complexity |
1030
|
| Defined Atom Stereocenter Count |
1
|
| SMILES |
C[C@H]1CN(CCN1C2=NC(=O)N(C3=NC(=C(C=C32)F)C4=C(C=CC=C4F)O)C5=C(C=CN=C5C(C)C)C)C(=O)C=C
|
| InChi Key |
NXQKSXLFSAEQCZ-SFHVURJKSA-N
|
| InChi Code |
InChI=1S/C30H30F2N6O3/c1-6-23(40)36-12-13-37(18(5)15-36)28-19-14-21(32)26(24-20(31)8-7-9-22(24)39)34-29(19)38(30(41)35-28)27-17(4)10-11-33-25(27)16(2)3/h6-11,14,16,18,39H,1,12-13,15H2,2-5H3/t18-/m0/s1
|
| Chemical Name |
6-fluoro-7-(2-fluoro-6-hydroxyphenyl)-1-(4-methyl-2-propan-2-ylpyridin-3-yl)-4-[(2S)-2-methyl-4-prop-2-enoylpiperazin-1-yl]pyrido[2,3-d]pyrimidin-2-one
|
| Synonyms |
Sotorasib; AMG510; AMG-510 racemate; AMG 510
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture. |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
DMSO: 3.9~100 mg/mL (6.9~178.4 mM)
Ethanol: ~100 mg/mL (~178.4 mM) |
|---|---|
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples.
Injection Formulations
Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline)(e.g. IP/IV/IM/SC) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). View More
Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] Oral Formulations
Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). View More
Oral Formulation 3: Dissolved in PEG400 (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.7838 mL | 8.9192 mL | 17.8383 mL | |
| 5 mM | 0.3568 mL | 1.7838 mL | 3.5677 mL | |
| 10 mM | 0.1784 mL | 0.8919 mL | 1.7838 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
|
|---|
AMG 510 inhibits ERK phosphorylation and growth of KRASG12C-mutant tumours in vivo.Nature. 2019 Nov;575(7781):217-223. |
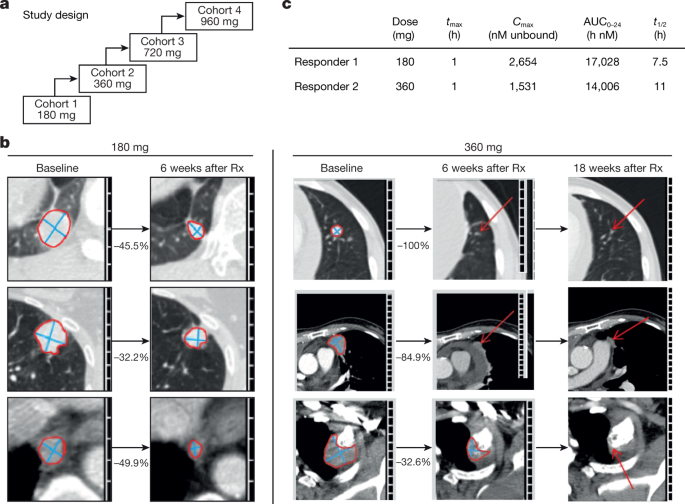 Clinical activity of AMG 510 in patients with lung cancer in first-in-human dose-escalation study.Nature. 2019 Nov;575(7781):217-223. Clinical activity of AMG 510 in patients with lung cancer in first-in-human dose-escalation study.Nature. 2019 Nov;575(7781):217-223. |