
| Size | Price | Stock | Qty |
|---|---|---|---|
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 2g | |||
| 5g | |||
| 10g | |||
| Other Sizes |
Purity: ≥98%
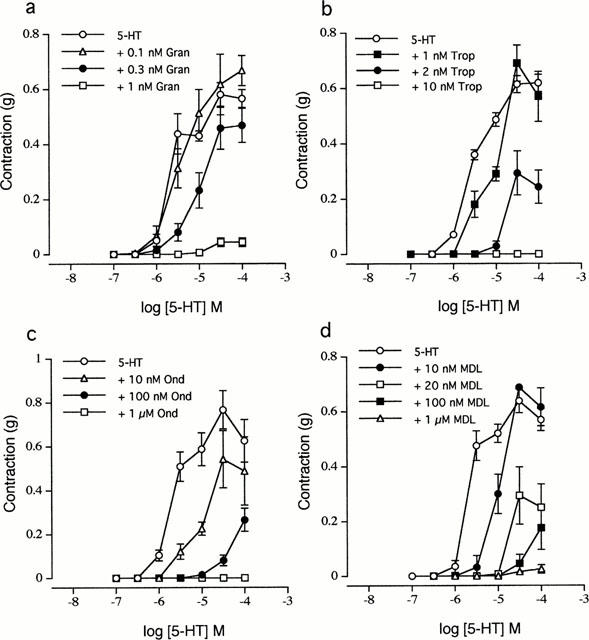
Ondansetron (GRC-50775; GR-38032; SN-307; GR38032; SN307; GR-C507/75; Zofran), an approved antiemetic drug, is a potent serotonin 5-HT3 receptor antagonist which is used to prevent nausea and vomiting caused by cancer chemotherapy, and radiation therapy. Ondansetron, a 5-HT3A receptor antagonist, reversibly inhibited the 5-HT (30 microM) signal by 70% at 0.3 nM and completely eliminated the response at 3 nM. The study found that auditory gating improved with 0.33 and 1 mg/kg, IP, but not with the lowest tested acute ondansetron dose of 0.1 mg/kg.
| Targets |
5-HT3
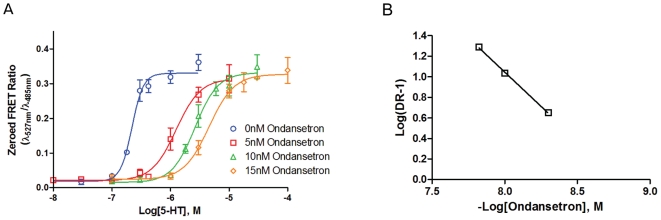
Ondansetron (GR 38032; SN 307; GR-C507/75) is a highly selective antagonist of the human 5-hydroxytryptamine 3 (5-HT3) receptor, with primary affinity for the 5-HT3A subtype: - Human recombinant 5-HT3A receptor: Ki = 0.6 nM (using [³H]-granisetron as the radioligand) [2] - Human recombinant 5-HT3A receptor: IC50 = 1.2 nM (inhibition of 5-HT-induced inward current, patch-clamp recording) [1] - No significant binding to other 5-HT receptor subtypes (5-HT1A/2A/2C/4/7, Ki > 1000 nM) or neurotransmitter receptors (e.g., dopamine D2, α1-adrenergic, histamine H1, Ki > 1000 nM) [1,2] |
|---|---|
| ln Vitro |
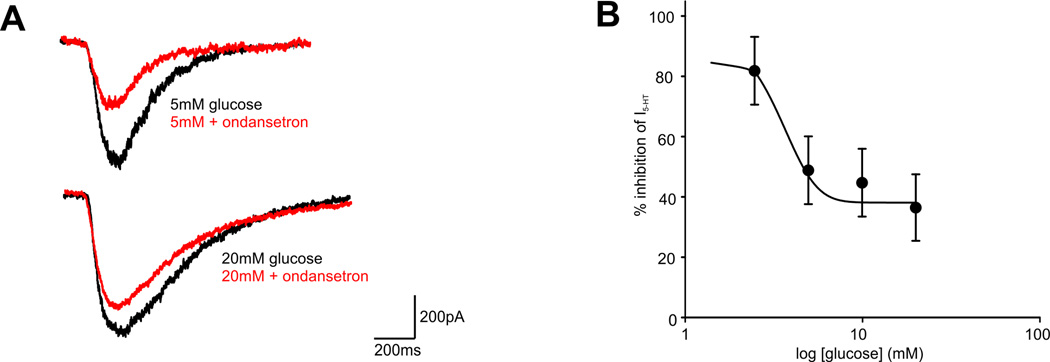
Inhibition of 5-HT3A receptor-mediated inward current: HEK293 cells expressing human 5-HT3A receptors were subjected to outside-out patch-clamp recording. Pretreatment with Ondansetron (0.1–10 nM) for 5 minutes inhibited 1 μM 5-HT-induced inward current in a dose-dependent manner. At 1 nM, current amplitude was reduced by 50% (IC50 = 1.2 nM); at 10 nM, inhibition reached >90% [1]
- Modulation of 5-HT3A receptor gating kinetics: In HEK293 cell outside-out patches, Ondansetron (0.5 nM) prolonged the deactivation time constant of 5-HT3A receptors from 12 ms (vehicle) to 28 ms, without affecting activation kinetics [2] - Anti-inflammatory effect on colonic epithelial cells: Primary rat colonic epithelial cells treated with Ondansetron (1–10 μM) for 24 hours showed reduced TNF-α (by 45% at 5 μM) and IL-6 (by 38% at 5 μM) secretion induced by TNBS (100 μg/mL) (ELISA detection) [8] |
| ln Vivo |
Ondansetron (GR 38032; SN 307) (2.4-6 mg/kg; intraperitoneal injection; six times in 15 days) has a TD50 value of 3.7±0.6 mg/kg and an LD50 of 4.6±0.5 mg/kg in mice [4]. Ondansetron (8 mg/kg; intraperitoneal injection; once) combined with olanzapine has a good effect in preventing CINV in patients with NSCLC, especially for advanced patients [7]. Ondansetron (2 mg/kg; intraperitoneal injection; six consecutive days) Animal model: NSCLC patients receiving chemotherapy [7] Dosage: 8 mg Administration method: intraperitoneal injection (ip) Results: showed TD50 and LD50 doses of 3.7± 0.6 mg) exhibits anti-inflammatory effects through 5-HT3 receptors [8]. They are 4.6±0.5 mg/kg and 4.6±0.5 mg/kg respectively. Animal model: Male Swiss mice with colitis [8] Dosage: 2 mg/kg Administration: intraperitoneal injection (ip) Results: Demonstrated MPO activity and tumor necrosis factor-α, interleukin-6 and leukocyte-interleukin 1β was significantly reduced.
Improved auditory gating in DBA/2 mice: Male DBA/2 mice (8–10 weeks old, 20–25 g) received intraperitoneal (i.p.) injection of Ondansetron (0.1, 0.5, 1 mg/kg) 30 minutes before the prepulse inhibition (PPI) test. At 0.5 mg/kg, PPI of the acoustic startle response increased by 32% (from 21% to 28%) vs. vehicle, which was blocked by the muscarinic antagonist scopolamine (1 mg/kg, i.p.), confirming a cholinergic mechanism [3] - Circadian variation in acute toxicity: Male ICR mice (20–25 g) were i.p. injected with Ondansetron (100–800 mg/kg) at two circadian time points (CT6: light phase; CT18: dark phase). LD50 was 620 mg/kg at CT6 and 480 mg/kg at CT18, with higher mortality (60% vs. 40% at 500 mg/kg) during the dark phase [4] - Blockade of ethanol-induced locomotor sensitization: Male C57BL/6 mice (6–8 weeks old) were treated with Ondansetron (0.1, 0.5 mg/kg, i.p.) 30 minutes before daily ethanol (2 g/kg, i.p.) administration for 7 days. After a 7-day withdrawal, the ethanol-induced increase in locomotor activity (sensitization) was reduced by 45% at 0.5 mg/kg vs. vehicle (open field test, 30-minute recording) [5] - Prevention of chemotherapy-induced nausea and vomiting (CINV): Female BALB/c nu/nu mice bearing A549 non-small cell lung cancer xenografts were randomized into 3 groups (n=8/group): 1. Vehicle + Cisplatin: Oral 0.5% CMC-Na + cisplatin (5 mg/kg, i.p., day 1); 2. Olanzapine + Cisplatin: Olanzapine (2 mg/kg, oral, daily) + cisplatin; 3. Olanzapine + Ondansetron + Cisplatin: Olanzapine (2 mg/kg, oral) + Ondansetron (0.5 mg/kg, i.p., day 1–3) + cisplatin. The combination group had 65% fewer vomiting episodes (1.2 vs. 3.4 in vehicle group) and 50% less weight loss (5% vs. 10%) over 7 days [7] - Attenuation of TNBS-induced colitis in rats: Male Wistar rats (250–300 g) received TNBS (100 mg/kg, 50% ethanol, intracolonic enema) to induce colitis, then Ondansetron (0.1, 0.5, 1 mg/kg, i.p.) daily for 7 days. At 0.5 mg/kg, colon length increased by 20% (from 12 cm to 14.4 cm), and myeloperoxidase (MPO) activity decreased by 35% vs. TNBS-only group [8] |
| Enzyme Assay |
Human 5-HT3A Receptor Binding Assay: The 200 μL reaction system contained 50 μg of membrane protein from HEK293 cells expressing human 5-HT3A receptors, 0.5 nM [³H]-granisetron (radioligand), and Ondansetron (0.01–100 nM). Incubated at 25°C for 60 minutes in 50 mM Tris-HCl (pH 7.4, 10 mM MgCl₂, 150 mM NaCl). Terminated by filtration through glass fiber filters pre-soaked in 0.3% polyethyleneimine. Filters washed 3× with cold buffer, radioactivity measured via liquid scintillation counter. Non-specific binding determined with 10 μM unlabeled granisetron; Ki calculated via Cheng-Prusoff equation [2]
- 5-HT3A Receptor Outside-Out Patch-Clamp Assay: HEK293 cells expressing human 5-HT3A receptors were cultured in DMEM + 10% FBS for 48 hours. Outside-out patches were excised using a glass pipette (3–5 MΩ resistance) filled with intracellular solution (140 mM KCl, 10 mM HEPES, 1 mM EGTA, pH 7.3). Ondansetron (0.1–10 nM) was added to the extracellular solution (140 mM NaCl, 5 mM KCl, 2 mM CaCl₂, 10 mM HEPES, pH 7.4) 5 minutes before application of 1 μM 5-HT. Current was recorded at -60 mV holding potential, and inhibition % was calculated vs. 5-HT-only current [1] |
| Cell Assay |
Primary Rat Colonic Epithelial Cell Inflammation Assay: Colonic epithelial cells were isolated from male Wistar rats, seeded in 24-well plates (5×10⁴ cells/well), and cultured in DMEM/F12 + 10% FBS for 24 hours. Cells were pretreated with Ondansetron (1–10 μM) for 1 hour, then stimulated with TNBS (100 μg/mL) for 24 hours. Culture supernatant was collected, and TNF-α/IL-6 levels were measured via sandwich ELISA. Cell viability was >90% at all Ondansetron concentrations (MTT assay) [8]
- HEK293-5-HT3A Cell Current Kinetics Assay: HEK293 cells expressing 5-HT3A receptors were seeded on coverslips, cultured for 48 hours. Whole-cell patch-clamp was performed with pipettes filled with intracellular solution (140 mM CsCl, 10 mM HEPES, 1 mM EGTA, pH 7.3). Ondansetron (0.5 nM) was added to extracellular solution, and 1 μM 5-HT was applied for 1 second. Activation (τₐ) and deactivation (τd) time constants were calculated by fitting current traces to a double-exponential model [2] |
| Animal Protocol |
NSCLC Patients Treated With Chemotherapy
8 mg Intraperitoneal Injection (i.p.) DBA/2 Mouse Auditory Gating Model: Male DBA/2 mice (8–10 weeks old, 20–25 g) housed at 22±2°C (12 h light/dark cycle) were randomized into 4 groups (n=8/group): 1. Vehicle: I.p. injection of 0.9% saline (10 mL/kg); 2. Ondansetron 0.1 mg/kg: I.p. injection of Ondansetron (0.1 mg/kg, dissolved in saline); 3. Ondansetron 0.5 mg/kg: I.p. injection of Ondansetron (0.5 mg/kg); 4. Ondansetron 0.5 mg/kg + Scopolamine: I.p. injection of Ondansetron (0.5 mg/kg) + scopolamine (1 mg/kg). Thirty minutes post-injection, PPI was measured: startle stimulus (120 dB, 40 ms) with/without prepulse (80 dB, 20 ms, 100 ms before startle). PPI % = [(startle without prepulse – startle with prepulse)/startle without prepulse] × 100 [3] - ICR Mouse Circadian Toxicity Model: Male ICR mice (6–8 weeks old, 20–25 g) entrained to 12 h light/dark cycle (lights on 06:00–18:00, CT0=lights on) for 2 weeks. Randomized into 8 groups (n=10/group) by circadian time (CT6/CT18) and Ondansetron dose (100–800 mg/kg, i.p., dissolved in saline). Mortality was recorded every 6 hours for 24 hours; LD50 calculated via Probit analysis [4] - C57BL/6 Mouse Ethanol Sensitization Model: Male C57BL/6 mice (6–8 weeks old) randomized into 3 groups (n=10/group): 1. Vehicle + Saline: I.p. saline + i.p. saline (daily, 7 days); 2. Vehicle + Ethanol: I.p. saline + i.p. ethanol (2 g/kg, daily, 7 days); 3. Ondansetron + Ethanol: I.p. Ondansetron (0.5 mg/kg) + i.p. ethanol (2 g/kg, daily, 7 days). After 7-day withdrawal, locomotor activity was recorded in open field (40×40 cm) for 30 minutes post-ethanol (2 g/kg, i.p.) [5] - Rat TNBS Colitis Model: Male Wistar rats (250–300 g) fasted for 24 hours, anesthetized with isoflurane. TNBS (100 mg/kg in 50% ethanol, 0.5 mL) was administered via intracolonic enema (5 cm from anus). Rats randomized into 4 groups (n=6/group): 1. Sham: Enema with 0.5 mL 50% ethanol + i.p. saline; 2. TNBS + Vehicle: TNBS + i.p. saline (daily, 7 days); 3. TNBS + Ondansetron 0.1 mg/kg: TNBS + i.p. Ondansetron (0.1 mg/kg, daily, 7 days); 4. TNBS + Ondansetron 0.5 mg/kg: TNBS + i.p. Ondansetron (0.5 mg/kg, daily, 7 days). On day 8, colon length was measured, and MPO activity (using o-dianisidine substrate) was assayed in colon homogenates [8] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion
Ondansetron is absorbed via the gastrointestinal tract and undergoes limited first-pass metabolism. In healthy subjects, the mean bioavailability after a single 8 mg tablet dose is approximately 56% to 60%. The presence of food slightly increases bioavailability. Systemic exposure to ondansetron increases disproportionately with dose. The AUC of the 16 mg tablet is 24% higher than the predicted value for the 8 mg tablet. This may reflect the reduced first-pass metabolism at higher oral doses. Following oral or intravenous administration, ondansetron is extensively metabolized and excreted in urine and feces. The volume of distribution of ondansetron is approximately 160 liters. The clearance of ondansetron in different age groups is approximately: 0.38 L/h/kg for healthy adult volunteers aged 19–40 years, 0.32 L/h/kg for healthy adult volunteers aged 61–74 years, and 0.26 L/h/kg for healthy adult volunteers ≥75 years. Ondansetron is a 5-HT3 receptor antagonist with good antiemetic activity in cats. This study aimed to evaluate the pharmacokinetics of ondansetron in healthy cats. Six cats with normal blood counts, serum biochemistry, and urinalysis results were crossover-designed and administered 2 mg of ondansetron orally (mean dose 0.43 mg/kg), subcutaneously (mean dose 0.4 mg/kg), and intravenously (mean dose 0.4 mg/kg), with a 5-day washout period between each administration route. Serum samples were collected before administration and at 0.25, 0.5, 1, 2, 4, 8, 12, 18, and 24 hours after administration. Ondansetron concentrations were determined using liquid chromatography-tandem mass spectrometry. Non-compartmental pharmacokinetic and dosing interval models were performed. Repeated measures ANOVA was used to compare parameters across different administration routes. The bioavailability of ondansetron was 32% orally and 75% subcutaneously. The elimination half-lives of ondansetron were calculated to be 1.84 ± 0.58 hours for intravenous injection, 1.18 ± 0.27 hours for oral administration, and 3.17 ± 0.53 hours for subcutaneous injection. The elimination half-life of subcutaneous ondansetron was significantly longer than that of oral or intravenous administration (P < 0.05). In healthy cats, subcutaneous ondansetron had higher bioavailability and longer drug exposure. This information is helpful in the treatment of vomiting in felines. Nausea and vomiting are among the major side effects of certain drug treatments (such as chemotherapy, radiotherapy, and general anesthesia). Due to the specific nature of these symptoms, oral administration is not appropriate, and intravenous injection may be impractical. This study aimed to develop a transdermal gel (2% Klucel) for ondansetron (a first-line 5-HT3 receptor antagonist antiemetic). First, we investigated the effects of the penetration enhancers camphor and isopropyl myristate (IPM) in vitro using a modified Franz diffusion cell. Then, we conducted in vivo experiments in a rabbit model by measuring skin and plasma concentrations. Due to the relatively long onset time of transdermal delivery, we tested the effect of microneedle roller skin treatment. In vitro penetration studies showed that the presence of 2.5% camphor or IPM increased steady-state flux by 1.2-fold and 2.5-fold, respectively, compared to the control gel. In vivo, ondansetron was not detected in either the skin or plasma after application of the matrix gel; however, the camphor gel and IPM gel delivered 20 and 81 μg/cm² of ondansetron, respectively. Microporization increased the plasma Cmax and AUC of the camphor gel by 10.47 ± 1.68-fold and 9.31 ± 4.91-fold, respectively, while the plasma Cmax and AUC of the IPM gel increased by 2.31 ± 0.53-fold and 1.59 ± 0.38-fold, respectively. In summary, the 2.5% IPM gel exhibited the best in vivo transdermal flux. Skin pretreatment with a microneedle roller slightly improved the delivery of isoproterenol gel and significantly enhanced the transdermal delivery of camphor gel. Ondansetron is a potent antiemetic commonly used to treat acute and chemotherapy-induced nausea and vomiting (CINV) in dogs. This study aimed to analyze the pharmacokinetics of ondansetron in dogs after a single oral dose. Eighteen beagle dogs were given a single oral dose of 8 mg ondansetron, and plasma ondansetron concentrations were determined by liquid chromatography-tandem mass spectrometry. Modeling analysis was performed using ADAPT5 software, and the model's discriminative power was determined by likelihood ratio test. The peak plasma concentration (Cmax) was 11.5 ± 10.0 ng/mL, and the time to peak concentration was 1.1 ± 0.8 hours. The area under the plasma concentration-time curve from time zero to the last measurable concentration was 15.9 ± 14.7 ng·hr/mL, and the half-life calculated from the terminal phase was 1.3 ± 0.7 hours. The pharmacokinetic parameters showed high inter-individual variability (coefficient of variation > 44.1%), and the one-compartment model effectively described the pharmacokinetics of ondansetron. Monte Carlo simulations estimated the commonly used empirical plasma concentration range to be 0.1–13.2 ng/mL. These results will help determine the optimal dosing regimen for chemotherapy-induced nausea and vomiting (CINV) in dogs. Ondansetron is the first-line drug for preventing nausea in women undergoing cesarean section and can also be used to prevent neonatal withdrawal syndrome (NAS). The pharmacokinetic characteristics of ondansetron in pregnant women or newborns are currently unknown. This study used a nonlinear mixed-effects model to analyze plasma samples from 20 non-pregnant women and 40 pregnant women after a single dose of 4 mg or 8 mg ondansetron, umbilical cord blood samples at delivery, and plasma samples from newborns after birth. Analysis showed that the distribution of ondansetron in vivo was not affected by pregnancy (P > 0.05), but was dose-dependent (P < 0.05). Furthermore, ondansetron exhibited rapid placental transport and a longer elimination half-life in newborns compared to mothers. Based on this model, a dosing regimen for the prevention of neonatal withdrawal syndrome (NAS) was designed. This regimen involved intravenous administration of 4 mg to the mother shortly before cord ligation, or oral administration of 0.07 mg/kg to the newborn (or an equivalent intravenous injection of 0.04 mg/kg). For more complete data on the absorption, distribution, and excretion of ondansetron (8 items in total), please visit the HSDB record page. Metabolism/Metabolites In vitro metabolic studies showed that ondansetron is a substrate of human hepatic cytochrome P450 enzymes, including CYP1A2, CYP2D6, and CYP3A4. CYP3A4 plays a major role in the overall metabolism of ondansetron. Because ondansetron is metabolized by multiple enzymes, the inhibition or absence of one enzyme (e.g., CYP2D6 deficiency) is likely to be compensated for by others, resulting in minimal change in the overall clearance of ondansetron. Following oral or intravenous administration, ondansetron is extensively metabolized and excreted in urine and feces. In humans, less than 10% of the dose is excreted unchanged in urine. The main urinary metabolites are glucuronide conjugates (45%), sulfate conjugates (20%), and hydroxylated products (10%). The primary metabolic pathway is hydroxylation of the indole ring, followed by glucuronide or sulfate conjugation. Although some unconjugated metabolites possess pharmacological activity, their plasma concentrations are insufficient to significantly affect the biological activity of ondansetron. Ondansetron is extensively metabolized in humans, with approximately 5% of the radiolabeled dose recovered in urine as the parent compound. Its primary metabolic pathway is hydroxylation of the indole ring, followed by glucuronide or sulfate conjugation. Although some unconjugated metabolites possess pharmacological activity, their plasma concentrations are insufficient to significantly affect the biological activity of ondansetron. Known metabolites of ondansetron include 6-hydroxyondansetron, 7-hydroxyondansetron, and 8-hydroxyondansetron. Liver function: Half-life: 5.7 hours. The half-life after oral or intravenous administration of 8 mg ondansetron is approximately 3-4 hours, which may be prolonged to 6-8 hours in elderly individuals. In humans… the elimination half-life is approximately 3-4 hours, but is prolonged in elderly patients. Six cats with normal complete blood counts, serum biochemistry, and urinalysis results received 2 mg orally (mean 0.43 mg/kg), subcutaneously (mean 0.4 mg/kg), and intravenously (mean 0.4 mg/kg), respectively. A crossover design was used, with a 5-day washout period, during which subjects were administered 0.4 mg/kg of ondansetron. Serum samples were collected before administration and at 0.25, 0.5, 1, 2, 4, 8, 12, 18, and 24 hours after administration. The elimination half-lives of ondansetron were calculated to be: 1.84 ± 0.58 hours for intravenous injection, 1.18 ± 0.27 hours for oral administration, and 3.17 ± 0.53 hours for subcutaneous administration. The elimination half-life of subcutaneous ondansetron was significantly longer than that of oral or intravenous administration (P < 0.05). … …Beagle dogs (n = 18) were given a single oral dose of 8 mg ondansetron, and the half-life calculated based on the terminal phase was 1.3 +/- 0.7 hours. ... Plasma protein binding rate: Ondansetron was 91% bound to human plasma (ultrafiltration, plasma concentration range: 0.1–10 μg/mL)[6] - Oral bioavailability: In male Sprague-Dawley rats, the oral bioavailability of ondansetron (10 mg/kg) was 60%, while that of intravenous (5 mg/kg) was 60%[6] - Plasma pharmacokinetics: In rats intravenously injected with 5 mg/kg ondansetron: Cmax = 2.5 μg/mL, Tmax = 5 min, elimination half-life (t1/2) = 3.2 h. Oral administration of 10 mg/kg: Cmax = 1.1 μg/mL, Tmax = 1.5 h, t1/2 = 3.8 h (HPLC-UV detection) [6] - Tissue distribution: Two hours after oral administration of 10 mg/kg ondansetron to mice, the highest drug concentrations were found in the liver (4.0 μg/g) and kidney (3.5 μg/g); the brain/plasma concentration ratio was 0.3 (low central nervous system penetration) [6] |
| Toxicity/Toxicokinetics |
Toxicity Summary
Identification and Uses: Ondansetron is crystallized from methanol. It is a drug used to prevent nausea and vomiting induced by highly emetogenic cancer chemotherapy in humans and veterinarians. QT interval prolongation and torsades de pointes have been reported in patients treated with ondansetron. Rare reports of liver failure and death have been found in cancer patients treated with ondansetron who are also taking other medications, including potentially hepatotoxic cytotoxic chemotherapy drugs and antibiotics. Ondansetron hydrochloride may cause serious allergic reactions. A study of children whose mothers took promethazine or ondansetron during pregnancy showed no clinically significant adverse neurobehavioral effects or obstetric outcomes. Another study indicated a low risk of teratogenicity with ondansetron, but it may increase the risk of cardiac septal defects. No evidence of genetic material damage was found in in vitro chromosomal aberration assays using human peripheral blood lymphocytes. Animal studies: Rats were orally administered ondansetron at doses of 1, 4, and 15 mg/kg during gametogenesis, mating, pregnancy, and lactation, respectively. Results showed that for F0 generation animals, the maximum ineffective dose of ondansetron for general toxicity and reproductive capacity was 4 mg/kg and 15 mg/kg, respectively. For F1 and F2 generation animals, the maximum ineffective dose for development was 15 mg/kg. During pregnancy and lactation, after daily intravenous administration of ondansetron at doses of 0.5, 1.5, and 4 mg/kg, results showed that for maternal rats, the maximum ineffective dose for general toxicity was 1.5 mg/kg; the maximum ineffective dose for maternal reproductive toxicity and for fetal and offspring developmental toxicity was 4 mg/kg. In rabbit intravenous organogenesis studies, mild maternal toxicity was observed in the highest dose group (4.0 mg/kg/day). Toxicity manifestations included decreased maternal weight and increased early fetal mortality. In vitro V-79 mammalian cell mutation studies and in vivo mouse bone marrow chromosomal aberration assays showed no evidence of genetic material damage. Microbial mutagenesis using mutant strains of Salmonella Typhimurium, Escherichia coli, or Saccharomyces cerevisiae (regardless of whether or not rat liver mitochondrial post-metabolic systems were used) showed no mutagenicity. No carcinogenicity was observed in 2-year oral administration of ondansetron at up to 10 mg/kg/day in rats and 30 mg/kg/day in mice, respectively. Ondansetron is a selective 5-HT3 receptor antagonist. Its antiemetic effect is achieved by inhibiting 5-HT3 receptors present in both the central (medullobulatory chemoreceptor area) and peripheral (gastrointestinal tract) regions. This inhibition of 5-HT3 receptors, in turn, inhibits visceral afferent stimulation of the vomiting center, possibly indirectly through the postmedullobulatory region or directly through inhibition of serotonin activity in the postmedullobulatory region and chemoreceptor trigger zone. Interactions: The nephrotoxicity of cisplatin limits its clinical application. Human organic cation transporter 2 (OCT2) and multidrug and toxin efflux proteins (MATEs) synergistically clear cationic drugs such as cisplatin from the kidneys. We hypothesized that ondansetron co-administration could affect cisplatin nephrotoxicity by altering the function of cisplatin transporters. In HEK-293 cells stably expressing OCT2 and MATEs, we determined the inhibitory efficacy of ondansetron on OCT2 and MATEs-mediated metformin accumulation. We investigated the effect of ondansetron on in vivo drug distribution by determining the pharmacokinetics of metformin (a classic substrate of OCT and MATEs) in wild-type and Mate1-/- mice. We evaluated the nephrotoxicity of wild-type and Mate1-/- mice after cisplatin treatment (with or without ondansetron). The results showed that MATEs, including human MATE1, human MATE2-K, and mouse Mate1, as well as OCT2 (in both humans and mice), were inhibited by ondansetron, with ondansetron exhibiting significantly greater inhibitory potency against MATEs than against OCT2. Ondansetron significantly increased tissue accumulation and pharmacokinetic exposure of metformin in wild-type mice (but not Mate1-/- mice). Furthermore, ondansetron treatment significantly enhanced cisplatin accumulation in the kidneys and cisplatin-induced nephrotoxicity, manifested by elevated levels of biochemical and molecular biomarkers and aggravated pathological histological changes in mice. Defects in mouse MATE functional genes also led to similar increases in nephrotoxicity. Therefore, the potent inhibitory effect of ondansetron on MATEs enhanced cisplatin-related nephrotoxicity in mice. The potential nephrotoxicity of combining the chemotherapy drug cisplatin with antiemetic 5-HT3 receptor antagonists (such as ondansetron) should be investigated in patients. While no pharmacokinetic interactions have been observed between ondansetron and tramadol, data from two small trials suggest that ondansetron may be associated with increased patient-controlled analgesia (PCA) with tramadol. Serotonin syndrome (including altered mental status, autonomic dysfunction, and neuromuscular abnormalities) has been reported with concomitant use of 5-HT3 receptor antagonists and other serotonergic drugs, including selective serotonin reuptake inhibitors (SSRIs) and serotonin and norepinephrine reuptake inhibitors. Treatment with potent CYP3A4 inducers (such as phenytoin sodium, carbamazepine, and others) should also be considered in patients receiving such agents. Ondansetron has a significantly increased clearance rate and lower plasma concentrations compared to rifampin. However, based on available data, dose adjustment of ondansetron is not recommended for patients taking these medications. For more complete data on interactions of ondansetron (8 items in total), please visit the HSDB record page. Non-human toxicity values Rat intravenous LD50 15-20 mg/kg Rat oral LD50 100-150 mg/kg Mouse intravenous LD50 1.0-2.5 mg/kg Mouse oral LD50 10-30 mg/kg Acute in vivo toxicity: As shown in the circadian rhythm study, the LD50 of ondansetron for intraperitoneal injection in male ICR mice was 620 mg/kg (CT6, during the day) and 480 mg/kg (CT18, during the night) [4] -Cardiotoxicity: In humans, ondansetron prolongs the QT interval by an average of 15 ms at the therapeutic dose (8 mg, intravenous). Patients with hypokalemia/hypomagnesemia or those taking other drugs that prolong the QT interval (e.g., clarithromycin) are at higher risk [6]. - Subacute toxicity: Rats were given ondansetron (10, 30, 100 mg/kg/day) orally for 28 days. No significant changes were observed in body weight (change <5%), serum ALT/AST/BUN/creatinine levels, or histopathological damage to the liver, kidneys, or heart [6]. |
| References |
|
| Additional Infomation |
Therapeutic Uses
/Clinical Trials/ ClinicalTrials.gov is a registry and results database that lists human clinical studies funded by public and private institutions worldwide. The website is maintained by the National Library of Medicine (NLM) and the National Institutes of Health (NIH). Each record on ClinicalTrials.gov includes a summary of the study protocol, including: the disease or condition; the intervention (e.g., the medical product, behavior, or procedure under investigation); the title, description, and design of the study; participation requirements (eligibility criteria); the location of the study; contact information for the study location; and links to relevant information from other health websites, such as the NLM's MedlinePlus (for providing patient health information) and PubMed (for providing citations and abstracts of academic articles in the medical field). Ondansetron is included in this database. Prevention of nausea and vomiting associated with highly emetogenic chemotherapy for cancer (including cisplatin)... /US product label includes/ Prevention of nausea and vomiting induced by initial and repeated courses of moderately emetogenic chemotherapy for cancer. /US Product Label Includes/ Prevention of nausea and vomiting during radiation therapy in patients receiving whole-body irradiation, a single high-dose abdominal irradiation, or daily fractionated abdominal irradiation. /US Product Label Includes/ For more complete data on the therapeutic uses of ondansetron (7 types), please visit the HSDB record page. Drug Warnings Ondansetron should be avoided in patients with congenital long QT syndrome due to the risk of QT interval prolongation. Electrocardiographic monitoring is recommended in patients with electrolyte abnormalities (such as hypokalemia or hypomagnesemia), congestive heart failure, or bradycardia, and in patients taking other medications known to prolong the QT interval. Electrolyte disturbances should be corrected before intravenous administration of ondansetron. Because the effect of ondansetron on the QT interval is dose-related, a single intravenous dose exceeding 16 mg should be avoided. Patients receiving ondansetron should seek immediate medical attention if they experience syncope, dizziness, arrhythmia, dyspnea, or vertigo. Based on reports of severe hypotension and loss of consciousness when apomorphine is used in combination with ondansetron, the combination of apomorphine and ondansetron is contraindicated. Patients should be informed that serotonin syndrome may occur when taking ondansetron and another serotonergic medication (such as medications for treating depression and migraines). Patients are advised to seek immediate medical attention if they experience the following symptoms: altered mental status, autonomic dysfunction, or neuromuscular symptoms with or without gastrointestinal symptoms. Rare reports of seizures (including tonic-clonic seizures) have been reported in patients taking ondansetron. For more complete data on ondansetron warnings (32 in total), please visit the HSDB record page. Pharmacodynamics Ondansetron is a highly specific and selective serotonin 5-HT3 receptor antagonist. It has not been shown to have activity against other known serotonin receptors and has a low affinity for dopamine receptors. 5-HT3 receptors for serotonin are located at peripheral vagal nerve endings and in the central postmedullar chemoreceptor trigger zone. The temporal relationship between the emetic effect of emetic drugs and serotonin release, as well as the efficacy of antiemetic drugs, suggests that chemotherapy drugs induce serotonin release from intestinal chromaffin cells by causing degenerative changes in the gastrointestinal tract. Serotonin then stimulates vagal and visceral receptors projecting to the medullary vomiting center, as well as 5-HT3 receptors in the postmedullar region, thereby initiating the vomiting reflex and causing nausea and vomiting. Furthermore, a double-blind, randomized, placebo- and positive-control (moxifloxacin) crossover study evaluated the effect of ondansetron on the QTc interval in 58 healthy adult men and women. This study tested single intravenous infusions of 8 mg and 32 mg ondansetron over 15 minutes. At the highest test dose of 32 mg, a prolonged Fridricia-corrected QTc interval (QT/RR0.33=QTcF) was observed from 15 minutes to 4 hours after infusion initiation, with the largest mean difference (upper limit of 90% CI) in baseline-corrected QTcF compared to placebo being 19.6 (21.5) ms, occurring at 20 minutes. At the lower test dose of 8 mg, a prolonged QTc interval was observed from 15 minutes to 1 hour after infusion initiation, with the largest mean difference (upper limit of 90% CI) in baseline-corrected QTcF compared to placebo being 5.8 (7.8) ms, occurring at 15 minutes. A greater degree of QTc interval prolongation is expected if ondansetron is infused at a rate exceeding 15 minutes. Intravenous administration of 32 mg ondansetron is contraindicated. No treatment-related changes in QRS duration or PR interval were observed at either the 8 mg or 32 mg dose. ECG evaluation studies of oral ondansetron have not yet been conducted. Based on a pharmacokinetic-pharmacodynamic model, assuming a mean peak plasma concentration of 24.7 ng/mL (95% CI 21.1, 29.0), an oral dose of 8 mg ondansetron is expected to result in a mean QTcF interval prolongation of 0.7 ms at steady state (90% CI -2.1, 3.3). The extent of QTc interval prolongation at the recommended dose of 5 mg/m² in pediatric patients has not been investigated, but the pharmacokinetic-pharmacodynamic model predicts a mean QTc interval prolongation of 6.6 ms at peak plasma concentrations (90% CI 2.8, 10.7). In healthy subjects, a single intravenous injection of 0.15 mg/kg ondansetron had no effect on esophageal motility, gastric motility, lower esophageal sphincter pressure, or small intestinal transit time. Multiple days of ondansetron administration have been shown to slow colonic transit in healthy subjects. Ondansetron has no effect on plasma prolactin concentration. Mechanism of action: Ondansetron (GR 38032; SN 307; GR-C507/75) mainly works by competitively antagonizing 5-HT3 receptors: 1. Blocks 5-HT-mediated activation of 5-HT3A receptors (ion channels), inhibiting the release of neurotransmitters in the gastrointestinal tract and chemoreceptor trigger zones (antiemetic effect) [1,6] 2. Enhances cholinergic transmission in the brain and improves auditory gating [3] 3. Reduces the release of pro-inflammatory cytokines (TNF-α, IL-6) and MPO activity, thereby alleviating colitis [8] - Therapeutic potential: Ondansetron has been clinically approved for the prevention of chemotherapy-induced nausea and vomiting (CINV), radiotherapy-induced nausea and vomiting, and postoperative nausea and vomiting (PONV). It has also shown potential for treating hearing gating disorders and inflammatory bowel disease (preclinical studies) [3,6,7,8] - FDA Warning: The FDA has issued a warning that ondansetron may cause QT interval prolongation, especially in patients with underlying heart disease or who are taking other QT prolonging medications [6] - Chemical Properties: Ondansetron (GR 38032; SN 307; GR-C507/75) is a white crystalline powder, soluble in DMSO (35 mg/mL) and slightly soluble in water (1.0 mg/mL). It is stable in aqueous solutions at pH 4.0–7.0 for 48 hours at room temperature [6] |
| Molecular Formula |
C18H19N3O
|
|---|---|
| Molecular Weight |
293.36
|
| Exact Mass |
293.152
|
| Elemental Analysis |
C, 73.69; H, 6.53; N, 14.32; O, 5.45
|
| CAS # |
99614-02-5
|
| Related CAS # |
Ondansetron hydrochloride dihydrate; 103639-04-9; Ondansetron-d5; 1219798-86-3; Ondansetron hydrochloride; 99614-01-4; Ondansetron-d3; 1132757-82-4; Ondansetron-13C,d3; 2699607-85-5
|
| PubChem CID |
4595
|
| Appearance |
White to off-white solid powder
|
| Density |
1.3±0.1 g/cm3
|
| Boiling Point |
546.0±30.0 °C at 760 mmHg
|
| Melting Point |
231 - 232ºC
|
| Flash Point |
284.0±24.6 °C
|
| Vapour Pressure |
0.0±1.5 mmHg at 25°C
|
| Index of Refraction |
1.678
|
| LogP |
2.07
|
| Hydrogen Bond Donor Count |
0
|
| Hydrogen Bond Acceptor Count |
2
|
| Rotatable Bond Count |
2
|
| Heavy Atom Count |
22
|
| Complexity |
440
|
| Defined Atom Stereocenter Count |
0
|
| SMILES |
O=C1C2C3=C([H])C([H])=C([H])C([H])=C3N(C([H])([H])[H])C=2C([H])([H])C([H])([H])C1([H])C([H])([H])N1C([H])=C([H])N=C1C([H])([H])[H]
|
| InChi Key |
FELGMEQIXOGIFQ-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C18H19N3O/c1-12-19-9-10-21(12)11-13-7-8-16-17(18(13)22)14-5-3-4-6-15(14)20(16)2/h3-6,9-10,13H,7-8,11H2,1-2H3
|
| Chemical Name |
9-methyl-3-[(2-methylimidazol-1-yl)methyl]-2,3-dihydro-1H-carbazol-4-one
|
| Synonyms |
GR 38032; SN 307; GR 38032F; GRC50775; GR-38032; SN-307; GR38032; SN307; GR-C507/75; trade name: Zofran
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: This product requires protection from light (avoid light exposure) during transportation and storage. |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
|
|||
|---|---|---|---|---|
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 1 mg/mL (3.41 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution.
For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 10.0 mg/mL clear DMSO stock solution to 400 μL of PEG300 and mix evenly; then add 50 μL of Tween-80 to the above solution and mix evenly; then add 450 μL of normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: 1 mg/mL (3.41 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), suspension solution; with ultrasonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 10.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. View More
Solubility in Formulation 3: ≥ 1 mg/mL (3.41 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.4088 mL | 17.0439 mL | 34.0878 mL | |
| 5 mM | 0.6818 mL | 3.4088 mL | 6.8176 mL | |
| 10 mM | 0.3409 mL | 1.7044 mL | 3.4088 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
Antiemetic Fosaprepitant To Remedy Nausea and Vomiting
CTID: NCT06382012
Phase: Phase 2/Phase 3 Status: Recruiting
Date: 2024-11-12
 |
|---|
 |
 |