
| Size | Price | Stock | Qty |
|---|---|---|---|
| 2mg |
|
||
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| Other Sizes |
Purity: ≥98%
Mitoglitazone (MSDC-0160; CAY10415), a thiazolidinedione analog,is the prototypical mTOT(mitochondrial target of thiazolidinediones)-modulating insulin sensitizer being investigated to treat diabetes and Alzheimer's disease. It is an insulin sensitizer free of side effects that are dependent on the peroxisome proliferator-activated receptor-γ (PPAR-γ). Insulin content is preserved and the resistance of the insulin-signaling pathway is decreased when islets are co-incubated with MSDC-0160 and IGF-1. Significantly reducing the loss of insulin content is also prevented by MSDC-0160 at 50μM. In addition, MSDC-0160 treatment results in AMPK phosphorylation being increased while mTOR phosphorylation is decreased. Furthermore, it is discovered that MSDC-0160 exhibits pro-survival effects in human islets by raising the expression of apoptosis-related genes like bcl2 and decreasing the amount of cleaved caspase-3.
| Targets |
mTOT
Mitochondrial pyruvate carrier (MPC) [2] - Peroxisome proliferator-activated receptor γ (PPARγ, indirect regulation,) [1] |
|---|---|
| ln Vitro |
MSDC-0160 restores IGF-1-induced Akt and GSK-3 phosphorylation and lessens resistance in the insulin/IGF-1 signaling pathway. When combined with IGF-1 and 8 mM glucose, MSDC-0160 elevates the expression of insulin, pdx1, nkx6.1, and nkx2.2 genes specific to β-cells and preserves insulin levels without affecting glucose-stimulated insulin secretion. Additionally, MSDC-0160 decreases the expression of apoptosis markers and increases human β-cell differentiation.[1]
In vitro culture of human islets, treatment with MSDC-0160 at 10 μM for 72 hours significantly increased glucose-stimulated insulin secretion (42% higher than the control group), and upregulated the mRNA and protein expressions of β-cell-specific markers PDX-1 and insulin (INS), maintaining β-cell phenotypic stability [1] - In human islets, MSDC-0160 regulated nutrient sensing pathways, significantly activating AMPK (the phosphorylation level of p-AMPKα Thr172 site increased by 2.3 times) and inhibiting the mTOR signaling pathway (the phosphorylation level of p-mTOR Ser2448 site decreased by 58%), improving islet cell energy metabolism [1] - In primary mouse cortical neurons, pretreatment with MSDC-0160 (5 μM, 24 hours) significantly alleviated MPP+-induced cell damage, increasing cell viability from 41% in the injured group to 68% and reducing lactate dehydrogenase (LDH) release by 35% [2] - In microglial cells (BV2 cell line), treatment with MSDC-0160 (1-10 μM) dose-dependently inhibited lipopolysaccharide (LPS)-induced inflammatory cytokine secretion. The mRNA expression levels of TNF-α and IL-6 were reduced by 62% and 55%, respectively, and autophagy activation was promoted (the LC3-II/LC3-I ratio increased by 2.1 times) [2] - In human islets, treatment with MSDC-0160 reduced the protein expressions of endoplasmic reticulum stress markers CHOP and GRP78 (by 40% and 38%, respectively) and decreased the β-cell apoptosis rate (from 12% in the control group to 6.5%) [1] |
| ln Vivo |
MSDC-0160 (100 mg/kg p.o.) improves insulin sensitivity by causing a significant drop in the product of circulating insulin and glucose in diabetic KKAy mice.
Mitochondrial and autophagic dysfunction as well as neuroinflammation are involved in the pathophysiology of Parkinson's disease (PD). We hypothesized that targeting the mitochondrial pyruvate carrier (MPC), a key controller of cellular metabolism that influences mTOR (mammalian target of rapamycin) activation, might attenuate neurodegeneration of nigral dopaminergic neurons in animal models of PD. To test this, we used MSDC-0160, a compound that specifically targets MPC, to reduce its activity. MSDC-0160 protected against 1-methyl-4-phenylpyridinium (MPP+) insult in murine and cultured human midbrain dopamine neurons and in an α-synuclein-based Caenorhabditis elegans model. In 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)-treated mice, MSDC-0160 improved locomotor behavior, increased survival of nigral dopaminergic neurons, boosted striatal dopamine levels, and reduced neuroinflammation. Long-term targeting of MPC preserved motor function, rescued the nigrostriatal pathway, and reduced neuroinflammation in the slowly progressive Engrailed1 (En1+/-) genetic mouse model of PD. Targeting MPC in multiple models resulted in modulation of mitochondrial function and mTOR signaling, with normalization of autophagy and a reduction in glial cell activation. Our work demonstrates that changes in metabolic signaling resulting from targeting MPC were neuroprotective and anti-inflammatory in several PD models, suggesting that MPC may be a useful therapeutic target in PD.[2] In the db/db diabetic mouse model, oral administration of MSDC-0160 at 30 mg/kg once daily for 4 weeks reduced fasting blood glucose from 28.5 mmol/L to 15.3 mmol/L, significantly improved glucose tolerance, and increased the insulin sensitivity index (ISI) by 65% [1] - In the diabetic mouse model, the number of pancreatic islet β-cells in the treatment group was 38% higher than that in the control group, the islet area was expanded by 45%, and the proportion of PDX-1-positive cells in the islets was increased, indicating improved β-cell function and survival [1] - In the MPTP-induced Parkinson's disease (PD) mouse model, intraperitoneal injection of MSDC-0160 at 10 mg/kg once daily for 14 days significantly improved motor dysfunction in mice (the rotarod test latency prolonged from 32 seconds to 68 seconds) [2] - In the PD mouse model, the loss rate of dopaminergic neurons in the substantia nigra pars compacta of the treatment group was reduced from 52% in the control group to 23%, the dopamine content in the striatum of the brain increased by 58%, and the expression of the microglial activation marker (Iba-1) was reduced by 42%, with alleviated inflammatory infiltration [2] |
| Enzyme Assay |
Even at 50μM, MSDC-0160 considerably reduces the loss of insulin content. Furthermore, treatment of MSDC-0160 decreases mTOR phosphorylation while increasing AMPK phosphorylation. Additionally, MSDC-0160 is discovered to exhibit pro-survival effects in human islets by upregulating the expression of genes linked to apoptosis, such as bcl2, and lowering the quantity of cleaved caspase-3.
Binding of MSDC-0160 to its Mitochondrial Target Protein (mTOT)[1] Human islets (∼1000–1500/sample) were homogenized, and 10 µg of protein (mitochondrial P2 fraction) was incubated with a 125I-labeled probe (MSDC-1101) that binds to Mpc2 with or without the concomitant addition of 20 µM MSDC-0160 as previously described. Mitochondrial pyruvate carrier (MPC) activity assay: Mouse liver mitochondria were isolated to prepare mitochondrial suspension. Radioactively labeled pyruvate substrate and gradient concentrations (0.1-20 μM) of MSDC-0160 were added. After incubation at 37℃ for 30 minutes, the radioactive intensity taken up by mitochondria was detected to calculate the pyruvate transport rate and the inhibitory rate of the drug on MPC [2] - AMPK kinase activity assay: After human islets were treated with MSDC-0160, total cellular protein was extracted and incubated with AMPK-specific substrate peptide and ATP in reaction buffer. After the reaction, the phosphorylation level of the substrate was detected to evaluate the change in AMPK kinase activity [1] - mTOR activity assay: The mTOR complex in islet cells was isolated by immunoprecipitation, and in vitro kinase reaction was performed by adding substrate protein and ATP. The phosphorylation degree of the substrate was detected by Western blot to analyze the inhibitory effect of MSDC-0160 on mTOR activity [1] |
| Cell Assay |
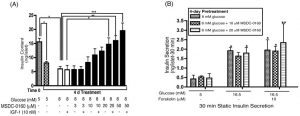
In human β-cells, MSDC-0160 inhibits nuclear translocation by localizing β-catenin on the cytoplasm or cell membrane. Islets were cultured in cCMRL with 8 mM glucose ± MSDC-0160 at 37°C. After 4 days, MSDC-0160 was removed and islets incubated for 90 min in cCMRL with 5 mM glucose. Insulin secretion was measured by static incubation for 30 min with cCMRL containing 5 or 16.5 mM glucose ± forskolin. Triplicate samples of 10 islets for each treatment were used. Media were collected and insulin determined by Human Insulin Specific RIA[1].
Human islet culture and function detection: Human islets were isolated from pancreatic tissue and seeded in culture plates coated with matrix. After incubation with 10 μM MSDC-0160 for 72 hours, the islets were stimulated with low glucose (2.8 mM) and high glucose (16.7 mM) respectively. The supernatant was collected to detect insulin secretion by ELISA; meanwhile, cellular RNA and protein were extracted to detect the expressions of PDX-1, INS, p-AMPK, and p-mTOR by RT-PCR and Western blot [1] - Neuronal damage protection assay: Primary mouse cortical neurons were seeded and pretreated with 5 μM MSDC-0160 for 24 hours, then MPP+ was added to induce cell damage. After 48 hours of culture, cell viability was detected by MTT assay, cytotoxicity by LDH kit, and neuronal morphology by immunofluorescence staining [2] - Microglial inflammation and autophagy detection: BV2 cells were seeded and incubated with gradient concentrations (1-10 μM) of MSDC-0160 for 1 hour, then stimulated with LPS for 24 hours. The supernatant was collected to detect inflammatory cytokine levels, and cellular protein was extracted to detect the expressions of autophagy markers such as LC3 and p62 by Western blot [2] - Islet cell apoptosis detection: After human islets were treated with MSDC-0160, the proportion of apoptotic cells was detected by flow cytometry with Annexin V/PI double staining; meanwhile, the expressions of endoplasmic reticulum stress-related proteins such as CHOP and GRP78 were detected by Western blot [1] |
| Animal Protocol |
Ten- to 12-week-old male C57BL/6J mice weighing 24 to 28 g
\n30 mg/kg \nOral gavage; daily; for 7 days \nC. elegans MPP+ neurodegeneration assay[2] \nWorms were synchronized, and L1 larvae (BY250 strain, GFP expression in dopaminergic neurons) were placed in 96-well plates containing OP50 bacteria in liquid culture (6 mg/ml) and MPP+ (0.75 mM) with MSDC-0160 (1, 10, or 100 μM). Wells containing no MPP+ [substituted with water or vehicle (methylcellulose)] and with MSDC-0160 alone were also included. Because in these experiments worms were soaked in solution containing MSDC-0160 of varying concentrations, the exact dose ingested by the worm cannot be accurately calculated. Therefore, the maximum concentration that had a neuroprotective effect was used in subsequent experiments to ensure efficacy. About 50 worms were added per well, and the plate was incubated at 20°C for 48 hours. After 48 hours, worms were moved and allowed to recover on unseeded nematode growth medium plates for several minutes before being mounted on an agarose pad with 3 mM levamisole and analyzed microscopically. Each worm was scored for the presence of GFP-fluorescent dopaminergic neurons in the anterior of the worm (CEP and ADE neurons). A minimum of 25 worms were analyzed for each condition in three independent trials.\n \nMeasurement of brain and plasma drug concentrations[2] \nC57BL/6J mice were orally dosed with MSDC-0160 (30 mg/kg) suspended in 1% low-viscosity methylcellulose with 0.01% Tween 80 in distilled water (10 ml/kg) and then euthanized 2 and 4 hours later. Plasma and whole-brain homogenates were extracted and subjected to LC/mass spectrometry measurement of both active drug and active alcohol metabolite (MSDC-0037), as previously described.\n \nMPTP mouse model[2] \nTen- to 12-week-old male C57BL/6J mice weighing 24 to 28 g were housed under standard conditions: constant temperature (22°C), humidity (relative, 30%), and a 12-hour light/dark cycle, with free access to food and water. Procedures were performed during daylight hours and were approved and supervised by the Institutional Animal Care and Use Committee at the Van Andel Research Institute. Mice were administered MSDC-0160 (30 mg/kg) by oral gavage beginning 24 hours before MPTP treatment. Next, mice received five consecutive doses of MPTP via intraperitoneal injection at 25 mg/kg per day (subacute regimen) along with coadministration of MSDC-0160, followed by 6 days of MSDC-0160 treatment. MSDC-0160 was dissolved in 1% methylcellulose with 0.01% Tween 80. Control mice received vehicle treatment (1% methylcellulose with 0.01% Tween 80). In the modest pathology stage, mice were administered MSDC-0160 (30 mg/kg per day) by oral gavage for 7 days starting 3 days after MPTP (25 mg/kg per day) treatment. Seven days after MPTP treatment, mice were euthanized, and tissues were processed for further evaluation. Mice were randomized to the experimental groups.\n \nEn1+/− mouse model[2] \nThe En1+/− heterozygous mice were maintained on an OF1 genetic background and under the same conditions as the C57BL/6J mice. In the mild pathology stage, En1+/− mice were fed a diet of chow formulated to deliver MSDC-0160 (30 mg/kg) starting at 3 weeks of age (at this point, no nigral cell death is detectable) and were euthanized at two different time points: 28 and 48 weeks. In the modest pathology stage, En1+/− mice were fed a diet of chow formulated to deliver v (30 mg/kg) starting at 8 weeks of age (at this point, 15 to 20% nigral cell death is detectable) and were euthanized at either 16 or 28 weeks. Mice were randomized to the groups, and control mice were fed regular chow. \nDiabetic mouse efficacy experiment: 6-week-old db/db mice were adaptively fed for 1 week and then randomly divided into a control group and a treatment group (8 mice per group). MSDC-0160 was dissolved in normal saline containing 0.5% sodium carboxymethylcellulose. The treatment group was given oral administration at 30 mg/kg every morning, and the control group was given an equal volume of vehicle for 4 consecutive weeks. Body weight and fasting blood glucose were monitored weekly during the experiment. A glucose tolerance test was performed at the end of administration, and pancreatic and liver tissues were collected after sacrificing the mice for subsequent detection [1] \n- Parkinson's disease mouse model experiment: 8-week-old C57BL/6 mice were randomly divided into a control group, a model group, and a treatment group (10 mice per group). The model group and the treatment group were injected with MPTP intraperitoneally to establish a PD model (once daily for 5 consecutive days). Starting from the 2nd day of modeling, the treatment group was injected with MSDC-0160 intraperitoneally (10 mg/kg, dissolved in 5% DMSO + normal saline) once daily for 14 consecutive days; the control group and the model group were given an equal volume of vehicle. Before the end of the experiment, the rotarod test was performed to evaluate motor function, and brain tissue was collected after sacrificing the mice for dopamine content detection and immunohistochemical analysis [2] |
| Toxicity/Toxicokinetics |
Four weeks after administration to diabetic mice, there were no significant differences in serum ALT, AST, creatinine, and blood urea nitrogen levels compared to the control group, and no obvious damage was observed in liver and kidney tissue pathological sections [1]. Fourteen days after administration to PD mice, there was no significant decrease in body weight (body weight change rate ≤3%), no toxic reactions such as diarrhea or tremors were observed, and no abnormal inflammation or necrosis was observed in brain tissue [2].
|
| References |
|
| Additional Infomation |
5-[[4-[2-(5-ethyl-2-pyridyl)-2-oxoethoxy]phenyl]methyl]thiazolidin-2,4-dione is an aromatic ether. Miglitol has been used in clinical trials investigating the treatment of type 2 diabetes and Alzheimer's disease. The main bottlenecks in human β-cell proliferation are limited proliferation, loss of β-cell phenotype, and increased apoptosis. In our previous studies, activation of the Wnt and mTOR signaling pathways significantly enhanced human β-cell proliferation. However, isolated human islets exhibited insulin signaling resistance, partly due to chronic activation of the mTOR/S6K1 signaling pathway leading to negative feedback in the insulin signaling pathway, as well as Akt phosphorylation and decreased insulin levels. We evaluated the effect of a novel insulin sensitizer, MSDC-0160, on restoring insulin/IGF-1 sensitivity and insulin levels in human β-cells. This novel thiazolidinedione (TZD) has low binding and activation affinity for PPARγ, exhibits insulin sensitization in a diabetic mouse model, and has shown glycemic reduction in a phase II clinical trial. MSDC-0160 treatment of human islets increased AMPK activity and decreased mTOR activity. This was associated with the restoration of IGF-1-induced Akt and GSK-3 phosphorylation and increased Pdx1 protein expression. Furthermore, MSDC-0160, in combination with IGF-1 and 8 mM glucose, increased the expression of β-cell-specific genes insulin, pdx1, nkx6.1, and nkx2.2, and maintained insulin levels without altering glucose-stimulated insulin secretion. Human islets cannot simultaneously promote DNA synthesis and maintain the β-cell phenotype. Lithium-induced GSK-3 inhibition promotes DNA synthesis, thereby blocking the ability of MSDC-0160 to maintain the β-cell phenotype. Conversely, MSDC-0160 inhibits the increase in DNA synthesis by blocking the nuclear translocation of β-catenin. Because these processes involve antagonistic pathways, we employed an in vitro sequential strategy to first induce human islet DNA synthesis, followed by MSDC-0160 to promote both β-cell phenotype and insulin levels. This new generation of PPARγ protective insulin sensitizer may provide a preliminary tool for alleviating the inherent insulin signaling pathway resistance of human islets, which is crucial for maintaining the β-cell phenotype during β-cell expansion, and thus has the potential to be used for the treatment of diabetes. [1] MSDC-0160 is a novel insulin sensitizer belonging to the thiazolidinedione derivatives. Unlike traditional thiazolidinedione drugs (such as rosiglitazone), MSDC-0160 does not directly activate PPARγ, but works by regulating mitochondrial metabolism and nutrient sensing pathways, thereby avoiding side effects such as weight gain. [1] The mechanism by which MSDC-0160 maintains the pancreatic β-cell phenotype is related to the activation of AMPK, inhibition of mTOR and reduction of endoplasmic reticulum stress, providing a new direction for islet protection therapy in type 2 diabetes. [1] In a Parkinson's disease model, MSDC-0160 exerts a neuroprotective effect by inhibiting MPC to regulate mitochondrial pyruvate metabolism, reducing neuronal damage, and inhibiting microglial activation and inflammatory response. [2] The dual action of MSDC-0160 (metabolic regulation, anti-inflammation, and neuroprotection) suggests its potential application value in metabolic-related neurodegenerative diseases. [1][2]
|
| Molecular Formula |
C19H18N2O4S
|
|---|---|
| Molecular Weight |
370.4222
|
| Exact Mass |
370.098
|
| Elemental Analysis |
C, 61.61; H, 4.90; N, 7.56; O, 17.28; S, 8.65
|
| CAS # |
146062-49-9
|
| Related CAS # |
1628078-14-7 (R-isomer);146062-49-9 (racemic);1628078-13-6 (S-isomer);
|
| PubChem CID |
10429242
|
| Appearance |
Off-white to light yellow solid powder
|
| Density |
1.3±0.1 g/cm3
|
| Boiling Point |
623.8±55.0 °C at 760 mmHg
|
| Flash Point |
331.1±31.5 °C
|
| Vapour Pressure |
0.0±1.8 mmHg at 25°C
|
| Index of Refraction |
1.619
|
| LogP |
2.84
|
| Hydrogen Bond Donor Count |
1
|
| Hydrogen Bond Acceptor Count |
6
|
| Rotatable Bond Count |
7
|
| Heavy Atom Count |
26
|
| Complexity |
534
|
| Defined Atom Stereocenter Count |
0
|
| SMILES |
S1C(N([H])C(C1([H])C([H])([H])C1C([H])=C([H])C(=C([H])C=1[H])OC([H])([H])C(C1C([H])=C([H])C(=C([H])N=1)C([H])([H])C([H])([H])[H])=O)=O)=O
|
| InChi Key |
IRNJSRAGRIZIHD-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C19H18N2O4S/c1-2-12-5-8-15(20-10-12)16(22)11-25-14-6-3-13(4-7-14)9-17-18(23)21-19(24)26-17/h3-8,10,17H,2,9,11H2,1H3,(H,21,23,24)
|
| Chemical Name |
5-[[4-[2-(5-ethylpyridin-2-yl)-2-oxoethoxy]phenyl]methyl]-1,3-thiazolidine-2,4-dione
|
| Synonyms |
Mitoglitazone; CAY10415; MSDC 0160; CAY 10415; MSDC-0160;CAY-10415; CAY 10415; CAY-10415; MSDC0160; CAY10415; 5-(4-(2-(5-ethylpyridin-2-yl)-2-oxoethoxy)benzyl)thiazolidine-2,4-dione; MSD-9;
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
DMSO: <1 mg/mL
Water: <1 mg/mL Ethanol: <1 mg/mL |
|---|---|
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution.
For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. View More
Solubility in Formulation 3: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6996 mL | 13.4982 mL | 26.9964 mL | |
| 5 mM | 0.5399 mL | 2.6996 mL | 5.3993 mL | |
| 10 mM | 0.2700 mL | 1.3498 mL | 2.6996 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT01374438 | Completed | Drug: MSDC-0160 Drug: Placebo |
Alzheimer's Disease | Metabolic Solutions Development Company |
July 2011 | Phase 2 |
| NCT00760578 | Completed | Drug: MSDC-0160 90 mg Drug: MSDC-0160 220 mg |
Type 2 Diabetes Mellitus | Metabolic Solutions Development Company |
September 2008 | Phase 2 |
| NCT01103414 | Completed | Drug: Mitoglitazone Drug: Pioglitazone |
Type 2 Diabetes | Metabolic Solutions Development Company |
September 2010 | Phase 2 |
 |
|---|
|
|