
| Size | Price | Stock | Qty |
|---|---|---|---|
| 500mg |
|
||
| 1g |
|
||
| 5g |
|
||
| 10g |
|
||
| Other Sizes |
Purity: =99.62%
Gefitinib (formerly ZD1839, ZD-1839 or trade name: Iressa) is a potent and orally bioavailable EGFR inhibitor with potential anticancer activity. In the NR6wtEGFR and NR6W cells, it inhibits EGFR Tyr1173, Tyr992, Tyr1173, and Tyr992 with IC50 values of 37 nM, 37 nM, 26 nM, and 57 nM, respectively. A variety of human tumor types, such as head and neck, prostate, breast, ovarian, colon, small-cell lung, and non-small-cell lung cancer, show anti-angiogenic properties when treated with gefitinib. The FDA authorized gefitinib in May 2003 for the treatment of non-small cell lung cancer (NSCLC). As a third-line therapy, it was authorized for use as monotherapy in patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) following the failure of both platinum-based and docetaxel chemotherapies.
| Targets |
Tyr1173 (IC50 = 26 nM); Tyr1173 (IC50 = 37 nM); Tyr992 (IC50 = 37 nM); Tyr992 (IC50 = 57 nM)
Gefitinib (ZD 1839) selectively inhibits epidermal growth factor receptor (EGFR) tyrosine kinase (IC₅₀ = 0.04 μM for recombinant EGFR kinase; IC₅₀ = 0.2 μM for EGFR phosphorylation in A431 cells) [2] Gefitinib (ZD 1839) shows no significant inhibition against other tyrosine kinases including c-Met, VEGFR2, and PDGFR (IC₅₀ > 100 μM) [4] |
|---|---|
| ln Vitro |
Gefitinib effectively inhibits all EGFR tyrosine phosphorylation sites in cell lines that express EGFR, including NR6, NR6M, and NR6W cell lines, as well as high and low-EGFR-expressing cell lines. Tyr992 and Tyr1173, two phosphorylation sites, are less sensitive and require greater concentrations of Gefitinib to inhibit. With an IC50 of 27 nM, gefitinib efficiently prevents PLC-γ phosphorylation in NR6W cells. PLC-γ phosphorylation is low in the NR6wtEGFR and NR6M cell lines, but it is more resistant to gefitinib inhibition in the latter, with IC50 values of 43 nM and 369 nM, respectively. Gefitinib inhibits Akt phosphorylations in the low-EGFR- and EGFRvIII-expressing cell lines, with IC50 values of 220 and 263 nM, respectively. When administered at doses ranging from 0.1 to 0.5μM, gefitinib significantly promotes NR6M cell colony formation as opposed to inhibiting it. On the other hand, Gefitinib totally prevents NR6M colony formation at a concentration of 2 μM. In both the high- and low-EGFR-expressing cell lines, gefitinib quickly and dose-dependently inhibits EGFR and ERK phosphorylation for up to 72 hours following EGF stimulation.[1] These EGF-driven untransformed MCF10A cells grow monolayerically when exposed to gefitinib, with an IC50 of 20 nM. [2] When paired with irradiation, Gefitinib (0.2 μM and 0.5 μM) significantly inhibited the growth of LoVo cells in comparison to radiation alone.[3]
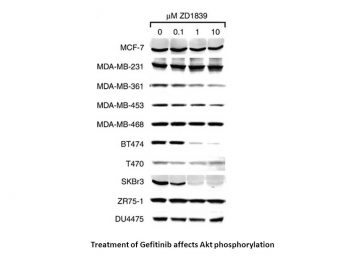
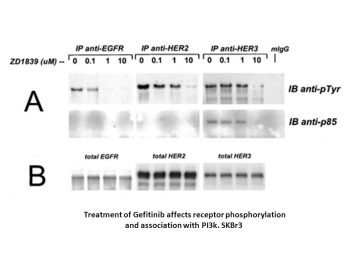
Epidermal growth factor receptor (EGFR) is frequently amplified and/or mutated in a number of human tumours and abnormal signalling from this receptor is believed to contribute to the malignant phenotype seen in these tumours. Gefitinib is a small molecule inhibitor that specifically binds and inhibits the EGFR tyrosine kinase and has been shown to inhibit the growth, proliferation, survival and invasion of a range of tumour cells overexpressing EGFR. However, clinical response to gefitinib has failed to correlate with EGFR levels and activity, indicating that other molecular mechanisms such as downstream signalling and mutations could be of importance in predicting clinical response. We therefore investigated the effect of the specific EGFR inhibitor gefitinib on the phosphorylation level, signalling and growth of cells expressing the naturally occurring constitutively active EGFR variant EGFRvIII, a low nontransforming level of EGFR and a high transforming level of EGFR. Results show that levels of gefitinib sufficient to suppress EGFR phosphorylations, EGFR-mediated proliferation and EGFR-mediated anchorage-independent growth are not sufficient to inhibit these features in cells expressing EGFRvIII. Furthermore, the data indicate that long-term exposure of EGFRvIII-expressing cells to low concentrations of gefitinib (0.01-0.1 microM) result in increased phosphotyrosine load of the receptor, increased signalling to ERK and stimulation of proliferation and anchorage-independent growth, presumably by inducing EGFRvIII dimerisation. Higher concentrations of gefitinib (1-2 microM), on the other hand, significantly decreased EGFRvIII phosphotyrosine load, EGFRvIII-mediated proliferation and anchorage-independent growth. Further studies are needed to investigate the implications of these important findings in the clinical setting.[1] The epidermal growth factor receptor (EGFR) is commonly overexpressed in many human tumors and provides a new target for anticancer drug development. ZD1839 (\"Iressa\"), a quinazoline tyrosine kinase inhibitor selective for the EGFR, has shown good activity in preclinical studies and in the early phase of clinical trials. However, because it remains unclear which tumor types are the best targets for treatment with this agent, the molecular characteristics that correlate with tumor sensitivity to ZD1839 have been studied. In a panel of human breast cancer and other epithelial tumor cell lines, HER2-overexpressing tumors were particularly sensitive to ZD1839. Growth inhibition of these tumor cell lines was associated with the dephosphorylation of EGFR, HER2, and HER3, accompanied by the loss of association of HER3 with phosphatidylinositol 3-kinase, and down-regulation of Akt activity. These studies suggest that HER2-overexpressing tumors are particularly susceptible to the inhibition of HER family tyrosine kinase signaling and suggest novel strategies to treat these particularly aggressive tumors.[2] Transforming growth factor alpha (TGF-alpha) is an autocrine growth factor for human cancer. Overexpression of TGF-alpha and its specific receptor, the epidermal growth factor receptor (EGFR), is associated with aggressive disease and poor prognosis. The EGFR has been proposed as a target for anticancer therapy. Compounds that block ligand-induced EGFR activation have been developed. ZD-1839 (Iressa) is a p.o.-active, quinazoline derivative that selectively inhibits the EGFR tyrosine kinase and is under clinical development in cancer patients. The antiproliferative activity of ZD-1839 alone or in combination with cytotoxic drugs differing in mechanism(s) of action, such as cisplatin, carboplatin, oxaliplatin, paclitaxel, docetaxel, doxorubicin, etoposide, topotecan, and raltitrexed, was evaluated in human ovarian (OVCAR-3), breast (ZR-75-1, MCF-10A ras), and colon cancer (GEO) cells that coexpress EGFR and TGF-alpha. ZD-1839 inhibited colony formation in soft agar in a dose-dependent manner in all cancer cell lines. The antiproliferative effect was mainly cytostatic. However, treatment with higher doses resulted in a 2-4-fold increase in apoptosis. A dose-dependent supra-additive increase in growth inhibition was observed when cancer cells were treated with each cytotoxic drug and ZD-1839. The combined treatment markedly enhanced apoptotic cell death induced by single-agent treatment. [4] Overexpression of the growth factor receptors EGFR and erbB2 occurs frequently in several human cancers and is associated with aggressive tumour behaviour and poor patient prognosis. We have investigated the effects of ZD1839 (Iressa), a novel EGFR tyrosine kinase inhibitor, on the growth, in vitro and in vivo, of human cancer cell lines expressing various levels of EGFR and erbB2. Proliferation of EGFR-overexpressing A431 and MDA-MB-231 cells in vitro was potently inhibited (50%-70%) by ZD1839 with half-maximally effective doses in the low nanomolar range. In parallel, ZD1839 blocked autophosphorylation of EGFR and prevented activation of PLC-gamma 1, ERK MAP kinases and PKB/Akt by EGF. It also inhibited proliferation in EGFR(+) cancer cell lines overexpressing erbB2 (SKBr3, SKOV3, BT474) by between 20% and 80%, effects which correlated with inhibition of EGF-dependent erbB2 phosphorylation and activation of ERK MAP kinase and PKB/Akt in SKOV3 cells.[6] Gefitinib (ZD 1839) dose-dependently inhibited the proliferation of EGFR-overexpressing tumor cell lines, including A431 (epidermoid carcinoma, IC₅₀ = 0.05 μM), NCI-H226 (non-small cell lung cancer, IC₅₀ = 0.12 μM), and MCF-7 (breast cancer, IC₅₀ = 0.3 μM). It blocked EGF-induced EGFR phosphorylation and downstream signaling (ERK1/2, Akt) in these cells at concentrations ≥ 0.1 μM [2] Gefitinib (ZD 1839) induced G1 phase cell cycle arrest and apoptosis in A431 cells. At 0.5 μM, it increased the proportion of apoptotic cells by ~40% and upregulated cleaved caspase-3 expression [5] Gefitinib (ZD 1839) suppressed the clonogenicity of NCI-H226 cells with an IC₅₀ of 0.08 μM. It also inhibited EGF-mediated cell migration in A549 lung cancer cells by ~65% at 0.2 μM [6] Gefitinib (ZD 1839) had no significant effect on the proliferation of EGFR-negative tumor cell lines (e.g., HT-29 colorectal cancer) at concentrations up to 10 μM [4] |
| ln Vivo |
Gefitinib (100 mg/kg) enhances radiation therapy's anti-tumor efficaciousness in LoVo tumor xenografts.[3] When established human GEO colon cancer xenografts are given to nude mice bearing these tumors, gefitinib treatment results in a reversible dose-dependent inhibition of tumor growth, as GEO tumors eventually resume the growth rate of controls.[4]
The effect of ZD1839 (‘Iressa’), a specific inhibitor of the tyrosine kinase activity of the epidermal growth factor receptor, on the radiation response of human tumour cells (LoVo colorectal carcinoma) was evaluated in vitro and in vivo. ZD1839 (0.5 μM, incubated days 1–5) significantly increased the anti-proliferative effect of fractionated radiation treatment (2 Gy day−1, days 1–3) on LoVo cells grown in vitro (P=0.002). ZD1839 combined with either single or fractionated radiotherapy in mice bearing LoVo tumour xenografts, also produced a highly significant increase in tumour growth inhibition (P⩽0.001) when compared to treatment with either modality alone. The radio-potentiating effect of ZD1839 was more apparent when radiation was administered in a fractionated protocol. This phenomenon may be attributed to an anti proliferative effect of ZD1839 on tumour cell re-population between radiotherapy fractions. These data suggest radiotherapy with adjuvant ZD1839 could enhance treatment response. Clinical investigation of ZD1839 in combination with radiotherapy is therefore warranted. [3] ZD-1839 treatment of nude mice bearing established human GEO colon cancer xenografts revealed a reversible dose-dependent inhibition of tumor growth because GEO tumors resumed the growth rate of controls at the end of the treatment. In contrast, the combined treatment with a cytotoxic agent, such as topotecan, raltitrexed, or paclitaxel, and ZD-1839 produced tumor growth arrest in all mice. Tumors grew slowly for approximately 4-8 weeks after the end of treatment, when they finally resumed a growth rate similar to controls. GEO tumors reached a size not compatible with normal life in all control mice within 4-6 weeks and in all single agent-treated mice within 6-8 weeks after GEO cell injection. In contrast, 50% of mice treated with ZD-1839 plus topotecan, raltitrexed, or paclitaxel were still alive 10, 12, and 15 weeks after cancer cell injection, respectively. These results demonstrate the antitumor effect of this EGFR-selective tyrosine kinase inhibitor and provide a rationale for its clinical evaluation in combination with cytotoxic drugs. [4] The blockade of epidermal growth factor receptor (EGFR) function with monoclonal antibodies has major antiproliferative effects against human tumors in vivo. Similar antiproliferative effects against some of these same tumors have also been observed with specific inhibitors of the EGFR-associated tyrosine kinase. One such inhibitor, the p.o. active ZD1839 (Iressa), has pronounced antiproliferative activity against human tumor xenografts. We now show that coadministration of ZD1839, as with anti-EGFR, will enhance the efficacy of cytotoxic agents against human vulvar (A431), lung (A549 and SK-LC-16 NSCL and LX-1), and prostate (PC-3 and TSU-PR1) tumors. Oral ZD1839 (five times daily x 2) and cytotoxic agents (i.p. every 3-4 days x 4) were given for a period of 2 weeks to mice with well-established tumors. On this schedule, the maximum tolerated dose (150 mg/kg) of ZD1839 induced partial regression of A431, a tumor that expresses high levels of EGFR, 70-80% inhibition among tumors with low but highly variable levels of EGFR expression (A549, SKLC-16, TSU-PR1, and PC-3), and 50-55% inhibition against the LX-1 tumor, which expresses very low levels of EGFR. ZD1839 was very effective in potentiating most cytotoxic agents in combination treatment against all of these tumors, irrespective of EGFR status, but dose reduction of ZD1839 below its single-agent maximum tolerated dose was required for optimum tolerance. The pronounced growth inhibitory action of the platinums, cisplatin and carboplatinum, as single agents against A431 vulvar, A549 and LX-1 lung, and TSU-PR1 and PC-3 prostate tumors was increased several-fold when ZD1839 was added, with some regression of A431 and PC-3 tumors. Although the taxanes, paclitaxel or docetaxel, as single agents markedly inhibited the growth of A431, LX-1, SK-LC-16, TSU-PR1, and PC-3, when combined with ZD1839, partial or complete regression was usually seen. Against A549, the growth inhibition of doxorubicin was increased 10-fold (>99%) with ZD1839. The folate analogue, edatrexate, was highly growth inhibitory against A549, LX-1, and TSU-PR1, whereas edatrexate combined with ZD1839 resulted in partial or complete regression in these tumors. Against the A431 tumor, paclitaxel alone either was highly growth inhibitory or induced some regression, but when combined with ZD1839, pronounced regression was obtained. Combination with gemcitabine neither added nor detracted from baseline cytotoxic efficacy, whereas ZD1839 combined with vinorelbine was poorly tolerated. Overall, these results suggest that potentiation of cytotoxic treatment with ZD1839 does not require high levels of EGFR expression in the target tumors. They also suggest significant clinical benefit from ZD1839 in combination with a variety of widely used cytotoxic agents [5]. Gefitinib (ZD 1839) inhibited tumor growth in nude mice bearing A431 xenografts when administered orally at 50 mg/kg/day for 21 days. Tumor volume was reduced by ~70% compared to the control group, and intratumoral EGFR phosphorylation was significantly downregulated [2] Gefitinib (ZD 1839) suppressed lung metastasis of B16-F10 melanoma cells (transfected with human EGFR) in C57BL/6 mice. Oral administration of 100 mg/kg/day for 14 days reduced the number of lung metastatic nodules by ~60% [3] In a phase I clinical study of patients with advanced solid tumors, Gefitinib (ZD 1839) (250-700 mg orally once daily) showed partial responses in 12% of patients, primarily in non-small cell lung cancer (NSCLC) [4] In patients with advanced NSCLC, Gefitinib (ZD 1839) (250 mg daily) resulted in a disease control rate (stable disease + partial response) of 42%, with a median progression-free survival of 2.8 months [6] |
| Enzyme Assay |
Gefitinib hydrochloride is an inhibitor with an IC50 value of 2-37 nM in NR6wtEGFR cells that selectively binds to and inhibits the EGFR tyrosine kinase. With an IC50 of 27 nM, gefitinib efficiently prevents PLC-γ phosphorylation in NR6W cells. PLC-γ phosphorylation is low in the NR6wtEGFR and NR6M cell lines, but it is more resistant to gefitinib inhibition in the latter, with IC50 values of 43 nM and 369 nM, respectively. Gefitinib inhibits Akt phosphorylations in the low-EGFR- and EGFRvIII-expressing cell lines, with IC50 values of 220 and 263 nM, respectively.
Crosslinking assay [1] Crosslinking of receptors were carried out as described (Montgomery, 2002). Briefly, Gefitinib-treated cells were washed twice in ice-cold phosphate-buffered saline (PBS) and solubilised in RIPA buffer containing protease and phosphatase inhibitors, 10% glycerol and 1 mM bis(sulfosuccinimidyl) suberate (BS3) for 20 min at 4°C. Glycine at a final concentration of 250 mM was subsequently added for 5 min, followed by centrifugation at 14 000 g for 10 min. Equivalent amounts of protein were resolved by SDS–PAGE and electroblotted onto nitrocellulose membranes. Blotting and antibody incubations were performed as above using anti-EGFR and antiphospho-tyrosine antibodies. Recombinant human EGFR kinase domain was incubated with ATP and a specific peptide substrate in the presence of serial dilutions of Gefitinib (ZD 1839). The reaction was conducted at 37°C for 60 minutes, and the phosphorylated substrate was detected using a radiometric assay. The inhibition rate was calculated by comparing the radioactivity with the vehicle control, and the IC₅₀ value was derived from the dose-response curve [2] To assess selectivity, the same protocol was used to test the inhibitory activity of Gefitinib (ZD 1839) against recombinant c-Met, VEGFR2, and PDGFR kinases. The reaction conditions were identical, and IC₅₀ values were determined to confirm selective targeting of EGFR [4] |
| Cell Assay |
Exponentially growing cells, such as NR6, NR6M, NR6M, and NR6W cells, are seeded in 96-well plates at a density of 2000 cells/well, allowed to adhere, and then washed in PBS before being incubated overnight in medium containing 0.5% FCS. After that, cells are exposed to different concentrations (0–2 μM) of either gefitinib or the solute controls, DMSO and EGF. Since NR6wtEGFR and NR6W cells can proliferate best at a known EGF concentration, 10 nM and 0.1 nM EGF, respectively, are added to NR6wtEGFR and NR6W cells. NR6 and NR6M cells do not receive additional EGF. An MTT proliferation assay is used to quantify the number of cells after 72 hours.
Proliferation assay [1] Exponentially growing cells were seeded in sextuple in 96-well plates at a concentration of 2000 cells/well, allowed to adhere and subsequently washed in PBS and incubated overnight in medium containing 0.5% FCS. Cells were then treated with varying concentrations of Iressa or the solute control DMSO and EGF. The optimal EGF concentration for inducing proliferation of NR6wtEGFR and NR6W cells has previously been determined and hence NR6wtEGFR and NR6W cells were added 10 and 0.1 nM EGF, respectively (Pedersen et al, unpublished observation). NR6 and NR6M cells were not added EGF. After 72 h the amount of cells were measured by performing a 3-[4,5-dimethylthiazol-2-yl]-2,5-diphenyltetrazolium bromide (MTT) proliferation assay. Soft agar assay for anchorage-independent growth [1] Exponentially growing cells (1 × 105) were suspended in 3 ml 0.5% (w/v) NuSieve low-melting agar dissolved in DMEM+0.5% FCS and plated in six-well plates covered with 0.5% agar dissolved in DMEM+0.5% FCS. Cells were then treated with varying concentrations of Iressa or the solute control DMSO. The optimal concentration of EGF for inducing anchorage-independent growth of NR6wtEGFR and NR6W cells has previously been determined and hence NR6wtEGFR were added 10 and 0.1 nM EGF, respectively (Pedersen et al, unpublished observation). NR6 and NR6M were not stimulated with EGF. Cultures in triplicate for each condition were replenished with fresh medium once a week. After 3 weeks the plates were stained with crystal violet and colonies >50 cells were counted. Analysis of proliferation in vitro [6] Cells (5 × 104) were plated in normal growth medium in triplicate into 24-well cell culture clusters. After 24 hr, cells were treated with Gefitinib or DMSO vehicle for a further 48 hr. Cells were then counted using a haemocytometer. Cell viability, assessed by trypan blue staining, was always ≥95% and did not alter with drug treatment. Proliferation was calculated as the increase in cell number during the 48 hr treatment period. Effects of ZD1839 are expressed relative to the increase in cell number observed in control cultures. All experiments were conducted on 3 separate occasions for each cell line. Analysis of apoptosis in vitro [6] Following treatment with Gefitinib, adherent cells were collected by trypsinisation and combined with nonadherent cells. Cells were washed and resuspended in PBS. Cell suspension (50 μl) was applied to a microscope slide using Cytospin 2. Cells were then fixed in paraformaldehyde and treated with Hoechst stain for 2 min. Apoptosis was then quantified by determining the proportion of cells containing nuclei with apoptotic morphology. One hundred cells were assessed in triplicate for each treatment. A431, NCI-H226, and MCF-7 cells were seeded in 96-well plates at 5×10³ cells/well and treated with Gefitinib (ZD 1839) (0.01-10 μM) for 72 hours. Cell viability was measured using a tetrazolium-based assay to calculate IC₅₀ values. For Western blot analysis, cells were treated with 0.1-1 μM gefitinib and stimulated with EGF, then lysed and probed with antibodies against phosphorylated EGFR, ERK1/2, Akt, and GAPDH [2] A431 cells were treated with Gefitinib (ZD 1839) (0.1-1 μM) for 24 hours. Cell cycle distribution was analyzed by flow cytometry after propidium iodide staining. Apoptosis was detected by Annexin V-FITC/PI staining, and cleaved caspase-3 expression was assessed by Western blot [5] NCI-H226 cells were seeded in 6-well plates at low density and treated with Gefitinib (ZD 1839) (0.01-0.5 μM) for 14 days. Colonies were fixed, stained, and counted to evaluate clonogenicity. A549 cells were used for migration assays in Boyden chambers, with 0.1-0.5 μM gefitinib treatment, and migrated cells were counted after 6 hours [6] |
| Animal Protocol |
Female nude mice (cba nu/nu) aged 8–10 weeks are intra-dermal injected with LoVo cells.
100 mg/kg Once daily by oral administration (0.1 mL/10 g body weight) for 14 days Growth of tumours in athymic mice and drug treatments [6] MDA-MB-231 or SKOV3 cells (2 × 106) in a 200 μl solution of 10% FCS with 50% (v/v) Matrigel were injected s.c. into each flank (2 tumours/mouse) of each mouse (n = 15) and allowed to form tumours over a period of 21 days. Mice were then gavaged daily with 75 mg/kg Gefitinib/ZD1839 or vehicle for 14 days. Tumour diameters were caliper-measured twice a week and tumour volume was calculated from the following formula: tumour volume = (width)2 × length/2. At the end of the experiment, tumours were removed from the mice, divided and processed for immunohistochemistry or stored in liquid nitrogen. The growth-inhibitory effect of Gefitinib/ZD1839 was calculated from the following formula: equation image, where d is final tumour volume after ZD1839 treatment, c is tumour volume before ZD1839 treatment, b is final tumour volume after control treatment and a is tumour volume before control treatment. Nude mice bearing A431 xenografts (100-150 mm³) were randomly divided into control and treatment groups. Gefitinib (ZD 1839) was suspended in 0.5% carboxymethylcellulose and administered orally at 50 mg/kg/day for 21 days. Tumor volume was measured every 3 days, and mice were euthanized to collect tumors for Western blot analysis of EGFR phosphorylation [2] C57BL/6 mice were injected with EGFR-transfected B16-F10 melanoma cells via the tail vein. Two days later, mice were treated with Gefitinib (ZD 1839) orally at 100 mg/kg/day for 14 days. Mice were euthanized, and lungs were harvested to count metastatic nodules under a microscope [3] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion
Absorption is slow after oral administration, with a mean bioavailability of 60%. Peak plasma concentrations occur 3–7 hours after administration. Food does not affect the bioavailability of gefitinib. Excretion is primarily via metabolism (mainly by CYP3A4) and feces. Excretion is primarily via feces (86%), with less than 4% of the administered dose excreted by the kidneys and its metabolites. Intravenous Dosage: 1400 L 595 mL/min Metabolism/Metabolites Mainly metabolized by hepatic CYP3A4. Three biotransformation sites have been identified: metabolism of the N-propoxymorpholine group, demethylation of the methoxy substituent on quinazoline, and oxidative defluorination of the halophenyl group. Known metabolites of gefitinib include O-demethylgefitinib and 4-defluoro-4-hydroxygefitinib. Biological half-life 48 hours [intravenous administration] Gefitinib (ZD 1839)The bioavailability of mice after a single oral dose of 50 mg/kg is approximately 59%. The plasma half-life is approximately 4.8 hours, and the maximum plasma concentration (Cmax) is 2.3 μg/mL 1 hour after administration [1] In rats, the 24-hour AUC₀-24h after oral administration of 100 mg/kg gefitinib (ZD 1839) is 28.6 μg·h/mL. The drug is widely distributed in the liver, lungs and tumor tissues, with a tumor-to-plasma concentration ratio of approximately 2.2 [3] In healthy volunteers, after oral administration of gefitinib (ZD 1839) (250 mg once daily), the Cmax was 1.9 μg/mL, the 24-hour AUC₀-24h was 19.1 μg·h/mL, and the plasma half-life was 14.7 hours. The drug is mainly metabolized by the liver, with 86% of the dose excreted in feces and 14% in urine within 7 days [4] |
| Toxicity/Toxicokinetics |
Hepatotoxicity
In early large clinical trials, 9% to 13% of patients receiving standard-dose gefitinib experienced elevated serum transaminase levels, and 2% to 4% had to discontinue treatment due to transaminase levels exceeding five times the upper limit of normal. Serum enzyme elevations typically appear after 4 to 12 weeks of treatment and are hepatocellular in nature. No reports of immune allergies or autoimmune features have been found, but skin rashes are common in patients receiving gefitinib. Most reported cases of gefitinib-induced liver injury are mild or asymptomatic and resolve within 1 to 2 months after discontinuation. Upon restarting treatment, serum enzyme levels typically (but not always) rise rapidly, and corticosteroid treatment does not appear to prevent this relapse. In some cases, patients can tolerate lower doses with mild or no ALT elevation. Regular monitoring of liver function is recommended during treatment. Although elevated serum transaminase levels are common during gefitinib treatment, clinically significant liver injury with jaundice is rare. The sponsor has received reports of severe and even fatal hepatotoxicity cases, therefore monitoring of liver function is recommended during treatment. Probability Score: B (May lead to clinically significant liver damage). Effects during Pregnancy and Lactation ◉ Overview of Use During Lactation There is currently no information on the clinical use of gefitinib during lactation. Because gefitinib binds to plasma proteins at a rate as high as 90%, its concentration in breast milk may be low. However, its half-life is approximately 48 hours, so it may accumulate in the infant. The manufacturer recommends discontinuing breastfeeding during gefitinib treatment. ◉ Effects on Breastfed Infants No published information found as of the revision date. ◉ Effects on Lactation and Breast Milk No published information found as of the revision date. Protein Binding 90% Primarily binds to serum albumin and α1-acid glycoprotein (regardless of drug concentration). Mice treated with gefitinib (ZD 1839) at a dose of 50 mg/kg/day for 21 days showed a slight decrease in body weight (approximately 8%), but no significant organ toxicity was observed. Serum alanine aminotransferase (ALT), aspartate aminotransferase (AST), and creatinine levels were all within the normal range [1]. In the Phase I clinical trial, the most common adverse events associated with gefitinib (ZD 1839) were rash (45%), diarrhea (30%), and nausea (20%). Grade 3/4 toxicities were rare, including severe diarrhea (3%) and elevated liver enzymes (2%) [5]. Gefitinib (ZD 1839) had a plasma protein binding rate of approximately 90% in human plasma as determined by balanced dialysis [6]. |
| References | |
| Additional Infomation |
Gefitinib belongs to the quinazoline class of compounds. Its structure is quinazoline, with (3-chloro-4-fluorophenyl)nitroso, 3-(morpholino-4-yl)propoxy, and methoxy groups substituted at positions 4, 6, and 7, respectively. It is an epidermal growth factor receptor (EGFR) kinase inhibitor used to treat non-small cell lung cancer. It has the effects of an EGFR antagonist and an anti-tumor drug. Gefitinib is an aromatic ether, belonging to the monochlorobenzene, monofluorobenzene, secondary amine, tertiary amine, quinazoline, and morpholine classes of compounds. Gefitinib (original code ZD1839) is a drug used to treat certain types of cancer. Its mechanism of action is similar to erlotinib (trade name: Tarceva), selectively targeting mutated proteins in malignant cells. Gefitinib is marketed by AstraZeneca under the brand name Iressa. Gefitinib is a kinase inhibitor. Its mechanism of action is as a protein kinase inhibitor. Gefitinib is a selective tyrosine kinase receptor inhibitor used to treat non-small cell lung cancer. Gefitinib treatment has been associated with transient elevations in serum transaminase levels and rare, clinically significant acute liver injury. Data on gefitinib infection with Penicillium brocae have been reported. Gefitinib is an aniline-quinazoline compound with antitumor activity. Gefitinib inhibits the catalytic activity of multiple tyrosine kinases, including the epidermal growth factor receptor (EGFR), which may lead to the inhibition of tyrosine kinase-dependent tumor growth. Specifically, the drug competitively binds to the tyrosine kinase domain of EGFR with ATP, thereby inhibiting receptor autophosphorylation and ultimately inhibiting signal transduction. Gefitinib may also induce cell cycle arrest and inhibit angiogenesis. (NCI04) A selective epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor used to treat locally advanced or metastatic non-small cell lung cancer. Drug Indications Gefitinib (Mylan) is indicated for the continued treatment of patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) who have failed platinum-based or docetaxel chemotherapy. FDA Label Gefitinib (Mylan) is indicated for monotherapy in adult patients with locally advanced or metastatic NSCLC harboring EGFR-TK activating mutations. Iressa (Iressa) is indicated for the treatment of adult patients with locally advanced or metastatic NSCLC harboring epidermal growth factor receptor tyrosine kinase activating mutations. Mechanism of Action Gefitinib is an epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor that binds to the enzyme's adenosine triphosphate (ATP) binding site. EGFR is frequently overexpressed in certain human cancer cells, such as lung and breast cancer cells. Overexpression leads to enhanced activation of the anti-apoptotic Ras signaling cascade, resulting in increased cancer cell survival and uncontrolled cell proliferation. Gefitinib is the first selective inhibitor of EGFR tyrosine kinase, also known as Her1 or ErbB-1. By inhibiting EGFR tyrosine kinase, downstream signaling cascades are also inhibited, thereby suppressing malignant cell proliferation. Pharmacodynamics Gefitinib inhibits intracellular phosphorylation of multiple tyrosine kinases associated with transmembrane cell surface receptors, including epidermal growth factor receptor (EGFR)-associated tyrosine kinase (EGFR-TK). EGFR is expressed on the cell surface of many normal and cancer cells. The epidermal growth factor receptor (EGFR) is frequently amplified and/or mutated in various human tumors, and aberrant signaling of this receptor is thought to be associated with the malignant phenotype of these tumors. Gefitinib is a small molecule inhibitor that specifically binds to and inhibits EGFR tyrosine kinase and has been shown to inhibit the growth, proliferation, survival, and invasion of various EGFR-overexpressing tumor cells. However, the lack of correlation between the clinical efficacy of gefitinib and EGFR levels and activity suggests that other molecular mechanisms, such as downstream signaling pathways and gene mutations, may play an important role in predicting clinical efficacy. Therefore, we investigated the effects of the specific EGFR inhibitor gefitinib on phosphorylation levels, signaling pathways, and growth in cells expressing the naturally occurring constitutively active EGFR variant EGFRvIII, low-level unconverted EGFR, and high-level converted EGFR. The results showed that gefitinib doses sufficient to inhibit EGFR phosphorylation, EGFR-mediated proliferation, and EGFR-mediated anchorage-independent growth were insufficient to inhibit these characteristics in EGFRvIII-expressing cells. Furthermore, the data indicated that long-term exposure of EGFRvIII-expressing cells to low concentrations of gefitinib (0.01–0.1 μM) led to increased receptor phosphotyrosine levels, enhanced ERK signaling, and stimulation of cell proliferation and anchorage-independent growth, likely through the induction of EGFRvIII dimerization. On the other hand, higher concentrations of gefitinib (1-2 μM) significantly reduced EGFRvIII phosphotyrosine levels and inhibited EGFRvIII-mediated cell proliferation and anchorage-independent growth. Further research is needed to explore the clinical significance of these important findings. [1] Epidermal growth factor receptor (EGFR) is widely overexpressed in many human tumors, providing a new target for the development of anticancer drugs. ZD1839 (Iressa) is a selective EGFR-targeting quinazoline tyrosine kinase inhibitor that has shown good activity in preclinical studies and early clinical trials. However, since it is not yet clear which tumor types are the best therapeutic targets for this drug, researchers have investigated the molecular characteristics associated with tumor sensitivity to ZD1839. Among a group of human breast cancer and other epithelial tumor cell lines, tumors overexpressing HER2 are particularly sensitive to ZD1839. Growth inhibition in these tumor cell lines is associated with dephosphorylation of EGFR, HER2 and HER3, accompanied by loss of HER3 binding to phosphatidylinositol 3-kinase and downregulation of Akt activity. These studies suggest that HER2-overexpressing tumors are particularly sensitive to inhibition of the HER family tyrosine kinase signaling pathway, and suggest new strategies for treating these highly aggressive tumors. [2] Transforming growth factor α (TGF-α) is an autocrine growth factor in human cancers. Overexpression of TGF-α and its specific receptor, epidermal growth factor receptor (EGFR), is associated with aggressive disease and poor prognosis. EGFR has been proposed as a target for anticancer therapy. Several compounds that can block ligand-induced EGFR activation have been developed. ZD-1839 (Iressa) is a pleiotropic quinazoline derivative that selectively inhibits EGFR tyrosine kinase and is currently being developed clinically in cancer patients. This study evaluated the antiproliferative activity of ZD-1839, alone or in combination with cytotoxic agents with different mechanisms of action (such as cisplatin, carboplatin, oxaliplatin, paclitaxel, docetaxel, doxorubicin, etoposide, topotecan, and raltitrexed), against human ovarian cancer (OVCAR-3), breast cancer (ZR-75-1, MCF-10A ras), and colon cancer (GEO) cells, all of which co-express EGFR and TGF-α. ZD-1839 inhibited colony formation in all cancer cell lines on soft agar in a dose-dependent manner. Its antiproliferative effect was primarily manifested as cell inhibition. However, higher doses increased apoptosis by 2–4-fold. When cancer cells were treated in combination with each cytotoxic agent and ZD-1839, a dose-dependent superadditive enhancement of growth inhibition was observed. Combination therapy significantly enhanced apoptosis induced by single-agent treatment. [4] Overexpression of growth factor receptors EGFR and erbB2 occurs frequently in various human cancers and is associated with tumor invasiveness and poor patient prognosis. We investigated the effects of a novel EGFR tyrosine kinase inhibitor, ZD1839 (Iressa), on the in vitro and in vivo growth of human cancer cell lines expressing different levels of EGFR and erbB2. ZD1839 effectively inhibited the in vitro proliferation of EGFR-overexpressing A431 and MDA-MB-231 cells at low nanomolar concentrations (inhibition rates of 50%-70%). Simultaneously, ZD1839 blocked EGFR autophosphorylation and inhibited EGF activation of PLC-γ1, ERK MAP kinase, and PKB/Akt signaling pathways. It can also inhibit the proliferation of EGFR(+) cancer cell lines (SKBr3, SKOV3, BT474) that overexpress erbB2, with inhibition rates ranging from 20% to 80%. This inhibitory effect is associated with the inhibition of EGF-dependent erbB2 phosphorylation and the activation of ERK MAP kinase and PKB/Akt in SKOV3 cells. Oral administration of ZD1839 can inhibit the growth of xenograft tumors MDA-MB-231 and SKOV3 established in athymic mice by 71% and 32%, respectively. Growth inhibition and proliferation reduction occur simultaneously, but the apoptosis index does not change. In summary, these results indicate that at the studied dose, ZD1839 can effectively inhibit not only the proliferation of EGFR-overexpressing cells, but also the proliferation of EGFR(+) cells that overexpress erbB2[6]. Gefitinib (ZD 1839) is a first-generation oral EGFR tyrosine kinase inhibitor that exerts its anti-tumor effect by blocking EGF-mediated EGFR activation and its downstream signaling pathways, thereby inhibiting tumor cell proliferation and inducing apoptosis [2]. Gefitinib (ZD 1839) has preferential efficacy against tumors with EGFR overexpression or activating mutations, especially non-small cell lung cancer [6]. The clinical activity of gefitinib (ZD 1839) in advanced solid tumors supports its status as a targeted therapy for EGFR-driven cancers [4].
|
| Molecular Formula |
C22H24CLFN4O3
|
|---|---|
| Molecular Weight |
446.90
|
| Exact Mass |
446.152
|
| Elemental Analysis |
C, 59.13; H, 5.41; Cl, 7.93; F, 4.25; N, 12.54; O, 10.74
|
| CAS # |
184475-35-2
|
| Related CAS # |
184475-35-2;857091-32-8; 184475-56-7; 184475-55-6; 1173976-40-3; 1173976-40-3; 1228664-49-0
|
| PubChem CID |
123631
|
| Appearance |
White solid powder
|
| Density |
1.3±0.1 g/cm3
|
| Boiling Point |
586.8±50.0 °C at 760 mmHg
|
| Melting Point |
119-1200C
|
| Flash Point |
308.7±30.1 °C
|
| Vapour Pressure |
0.0±1.6 mmHg at 25°C
|
| Index of Refraction |
1.621
|
| LogP |
4.11
|
| Hydrogen Bond Donor Count |
1
|
| Hydrogen Bond Acceptor Count |
8
|
| Rotatable Bond Count |
8
|
| Heavy Atom Count |
31
|
| Complexity |
545
|
| Defined Atom Stereocenter Count |
0
|
| SMILES |
ClC1=C(C([H])=C([H])C(=C1[H])N([H])C1C2C(=C([H])C(=C(C=2[H])OC([H])([H])C([H])([H])C([H])([H])N2C([H])([H])C([H])([H])OC([H])([H])C2([H])[H])OC([H])([H])[H])N=C([H])N=1)F
|
| InChi Key |
XGALLCVXEZPNRQ-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C22H24ClFN4O3/c1-29-20-13-19-16(12-21(20)31-8-2-5-28-6-9-30-10-7-28)22(26-14-25-19)27-15-3-4-18(24)17(23)11-15/h3-4,11-14H,2,5-10H2,1H3,(H,25,26,27)
|
| Chemical Name |
N-(3-chloro-4-fluorophenyl)-7-methoxy-6-(3-morpholin-4-ylpropoxy)quinazolin-4-amine
|
| Synonyms |
Gefitinib; ZD-1839; ZD1839; ZD 1839; Brand name: Iressa
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
|
|||
|---|---|---|---|---|
| Solubility (In Vivo) |
|
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.2376 mL | 11.1882 mL | 22.3764 mL | |
| 5 mM | 0.4475 mL | 2.2376 mL | 4.4753 mL | |
| 10 mM | 0.2238 mL | 1.1188 mL | 2.2376 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
| NCT Number | Recruitment | interventions | Conditions | Sponsor/Collaborators | Start Date | Phases |
| NCT03292133 | Active Recruiting |
Drug: EGF816 Drug: Gefitinib |
Lung Cancer | Massachusetts General Hospital | October 31, 2017 | Phase 2 |
| NCT03122717 | Active Recruiting |
Drug: Gefitinib Drug: Osimertinib |
Non-Small Cell Lung Cancer | Dana-Farber Cancer Institute | May 9, 2017 | Phase 1 Phase 2 |
| NCT03758287 | Active Recruiting |
Drug: Gefitinib Drug: CT053PTSA |
Non-small Cell Lung Cancer | Sunshine Lake Pharma Co., Ltd. | November 2016 | Phase 1 Phase 2 |
| NCT03849768 | Active Recruiting |
Drug: Gefitinib Drug: HS-10296 |
Non Small Cell Lung Cancer | Jiangsu Hansoh Pharmaceutical Co., Ltd. |
February 1, 2019 | Phase 3 |
| NCT02856893 | Active Recruiting |
Drug: Gefitinib Drug: Osimertinib |
NSCLC | European Organisation for Research and Treatment of Cancer - EORTC |
October 10, 2017 | Phase 2 |
A, effect of metformin (MET) alone and in combination with gefitinib (GEF) on cell proliferation, on anchorage-independent growth ability of NSCLC cell lines, and on the induction of apoptosis in CALU-3, CALU-3 GEF-R, and H1299 cell lines.Clin Cancer Res.2013 Jul 1;19(13):3508-19. |
Effects on the downstream pathway by combined treatment of metformin and gefitinib. Western blotting of EGFR, MAPK, AKT p70S6K, and S6 activation following treatment with the indicated concentration of metformin and gefitinib in CALU-3 and CALU-3 GEF-R cell lines. β-Actin was included as a loading control.Clin Cancer Res.2013 Jul 1;19(13):3508-19. |
Effects of the combination treatment of metformin and gefitinib on NSCLC tumor xenografts.Clin Cancer Res.2013 Jul 1;19(13):3508-19. |
 |
 |