
| Size | Price | Stock | Qty |
|---|---|---|---|
| 5mg |
|
||
| 10mg |
|
||
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg | |||
| Other Sizes |
Purity: ≥98%
BTZ043 racemate, the racemic mixture (R- and S-isomer) of BTZ043, is a decaprenylphosphoryl-β-D-ribose 2'-epimerase (DprE1) inhibitor acting as a new antimycobacterial agent that kill Mycobacterium tuberculosis. BTZ043 displayed similar activity against all clinical isolates of M. tuberculosis that were tested, including extensively drug-resistant and multidrug-resistant strains, indicating that it targets a previously unknown biological function. BTZ043 is bactericidal, reducing viability in vitro by more than 1000-fold in under 72 hours, which is comparable to the INH killing effect. It has potential to be used as a antimycobacterial agent that kill Mycobacterium tuberculosis by blocking arabinan synthesis. The inhibition of BTZ-resistant DprE1 followed the trend observed in the MIC measurements, with the C387G mutant being more resistant to inhibition by PyrBTZ01, PyrBTZ02, and BTZ043 (7- to 9-fold increases in IC50) than the C387S mutant (2.5- to 4-fold increases in IC50). Structure-activity relationship (SAR) studies revealed the 8-nitro group of the BTZ scaffold to be crucial for the mechanism of action, which involves formation of a semimercaptal bond with Cys387 in the active site of DprE1. BTZ043 presented favorable in vitro absorption-distribution-metabolism-excretion/toxicity (ADME/T) and in vivo pharmacokinetic profiles. BTZ043 did not show efficacy in a mouse model of acute tuberculosis, suggesting that BTZ-mediated killing through DprE1 inhibition requires a combination of both covalent bond formation and compound potency.
| Targets |
DprE1
|
||
|---|---|---|---|
| ln Vitro |
By targeting decaprenylphosphoryl-β-D-ribose 2-epimerase, BTZ043 abolishes the formation of decaprenylphosphoryl arabinose, leading to cell lysis and death of Mycobacterium tuberculosis. BTZ043 displays similar activity against all clinical isolates of M. tuberculosis, including multidrug-resistant and extensively drug-resistant strains. BTZ043 displays significant activity against M. tuberculosis H37Rv and Mycobacterium smegmatis with MIC of 1 ng/mL (2.3 nM) and 4 ng/mL (9.2 nM), respectively, which is more potent than those of the existing tuberculosis (TB) drugs isoniazid (INH) and ethambutol (EMB) with MIC of 0.02-0.2 μg/mL and 1-5 μg/mL, respectively. BTZ043 is less effective in two different model systems (auxotrophy and starvation) involving metabolically inert M. tuberculosis, indicating that BTZ043 blocks a step in active metabolism similar to isoniazid (INH). BTZ043 treatment in M. smegmatis cells decreases the growth rate rapidly followed by a swelling of the poles and lysis of the cells after a few hours, which is similar but delayed in M. tuberculosis. BTZ043 (1/4 MIC 0.375 ng/mL) in combination with TMC207 (1/4 MIC 20 ng/mL) has a stronger cidal effect on M. tuberculosis but not BTZ-resistant M. tuberculosis mutant than TMC207 alone at a concentration of 80 ng/mL.
The minimal inhibitory concentrations (MICs) of a variety of BTZs against different mycobacteria were very low, ranging from ~0.1 to 80 ng/ml for fast growers and from 1 to 30 ng/ml for members of the M. tuberculosis complex. The MIC of BTZ043 against M. tuberculosis H37Rv and Mycobacterium smegmatis were 1 ng/ml (2.3 nM) and 4 ng/ml (9.2 nM), respectively (Table 1), which compares favorably with those of the existing TB drugs isoniazid (INH) (0.02 to 0.2 μg/ml) and ethambutol (EMB) (1 to 5 μg/ml). From structure activity relationship studies, >30 different BTZ derivatives showed MICs of <50 ng/ml against tubercle bacilli (examples are shown in table S2). Crucially, BTZ043 displayed similar activity against all clinical isolates of M. tuberculosis that were tested, including multidrug-resistant and extensively drug-resistant strains, indicating that it targets a previously unknown biological function (table S3). BTZ043 is bactericidal, reducing viability in vitro by more than 1000-fold in under 72 hours (Fig. 1B), which is comparable to the killing effect seen with INH. In two different model systems (auxotrophy and starvation) involving metabolically inert M. tuberculosis, BTZ043 was less effective, which implies that it blocks a step in active metabolism, similar to INH [3]. |
||
| ln Vivo |
At the used concentrations, four weeks of BTZ043 treatment reduces the bacterial burden in the spleen and lungs by one and two logs, respectively. Further findings imply that BTZ043's effectiveness is dependent on time as opposed to dose. After a month, acute (5 g/kg) and chronic (25 and 250 mg/kg) toxicology studies in uninfected mice demonstrate that there are no negative anatomical, behavioral, or physiological effects, even at the highest dose tested.[3]
Effect of BTZs in the mycetoma animal model [1] When PBTZ169 and BTZ043 were administered at 100 mg/kg twice daily by gavage (Fig 4), only the former showed a statistically significant effect compared to the saline control (P = 0.017). No significant difference was detected in the BTZ043-treated group (P = 0.667). The mouse group treated with SXT showed a statistically significant difference compared to the control group (P = 0.007). Benzothiazinones are highly potent drug candidates for the treatment of tuberculosis and other actinobacterial infections. Because of the nanomolar activity of benzothiazinones, we expected excellent in vivo activity. At 100 mg/kg twice daily, we observed a therapeutic effect, but only with PBTZ169. In M. tuberculosis, a microorganism with a thicker and more hydrophobic cell-wall than N. brasiliensis, BTZ043 at 50 mg/kg once daily resulted in a significant decrease in the lung and spleen bacterial burden. PBTZ169 is a more effective drug, and in the mouse model of infection, it significantly decreases the amount bacilli at 25 mg/kg once daily compared with BTZ043 [1]. PyrBTZ01 is not active in a mouse model of acute TB. Given the encouraging ADME/T and PK data obtained for PyrBTZ01, we performed an in vivo efficacy study using a mouse model of acute TB. Mice were infected by intravenous injection of M. tuberculosis H37Rv and then treated with PyrBTZ01 (50 mg/kg) or isoniazid (25 mg/kg) once daily, by gavage, 5 days/week for 4 weeks. At the end of the experiment, CFU counts in the lungs were determined. While isoniazid and BTZ043 were effective, leading to ∼3.2-log-unit decreases in the numbers of CFU over 4 weeks, compared to the untreated control group, PyrBTZ01 did not provide any protection to the treated mice, and their microbiological and pathological responses were the same as those of the untreated animals [2]. The in vivo efficacy of BTZ043 was assessed 4 weeks after a low-dose aerosol infection of BALB/c mice in the chronic model of TB. Four weeks of treatment with BTZ043 reduced the bacterial burden in the lungs and spleens by 1 and 2 logs, respectively, at the concentrations used (Fig. 1D). Additional results suggest that BTZ efficacy is time- rather than dose-dependent. Acute (5 g/kg) and chronic (25 and 250 mg/kg) toxicology studies in uninfected mice showed that, even at the highest dose tested, there were no adverse anatomical, behavioral, or physiological effects after one month (table S5).[3] |
||
| Enzyme Assay |
BTZ043, also known as 8-Nitro-benzothiazinones (BTZs), is a potent inhibitor of decaprenyl-phosphoribose-epimerase (DprE1) with MIC values of of 2.3 nM and 9.2 nM for M. tuberculosis H37Rv and Mycobacterium smegmatis, respectively.
MIC determination for BTZ169 [1] We used the broth microdilution method based on the CLSI M24-A document that we previously described. As external controls, we used Escherichia coli ATCC 25922 and Staphylococcus aureus ATCC 29213. Because of the high susceptibility of Nocardiae, the concentrations ranged from 0.125 μg/mL to 0.0002 μg/mL. Drug susceptibility testing. [2] The in vitro activities against all mycobacterial strains were measured with the resazurin reduction microplate assay (REMA), by 2-fold serial dilution of the compounds in the working bacterial culture in 96-well plates (final volume of 100 μl). For M. tuberculosis and Mycobacterium bovis BCG, the plates were incubated for 1 week at 37°C; for Mycobacterium smegmatis strains, the incubation time was 24 h. Bacterial viability was determined by adding sterile resazurin (10 μl, 0.025% [wt/vol]), incubating the mixture, and measuring resazurin turnover by fluorescence (excitation wavelength, 560 nm; emission wavelength, 590 nm), using a Tecan Infinite M200 microplate reader. DprE1 assays. [2] The C387G and C387S mutant DprE1 proteins were generated using the pET28a-M. tuberculosis DprE1 plasmid and the QuikChange site-directed mutagenesis kit (Agilent), with the primers 5′-GGCTGGAACATCGGCGTCGACTTCCCC-3′ and 3′-CCGACCTTGTAGCCGCAGCTGAAGGGG-5′ (C387G) and 5′-GGCTGGAACATCAGCGTCGACTTCCCC-3′ and 3′-CCGACCTTGTAGTCGCAGCTGAAGGGG-5′ (G387S) (mutated bases are underlined). Wild-type M. tuberculosis DprE1 and the mutant enzymes were expressed and purified as described elsewhere. The 50% inhibitory concentrations (IC50s) for DprE1 were determined as described previously, using a coupled Amplex Red/horseradish peroxidase assay, with farnesyl-phosphoryl-β-d-ribofuranose (FPR) as the substrate. The conversion of Amplex Red to resorufin was followed by fluorescence measurements (excitation wavelength, 560 nm; emission wavelength, 590 nm) on a Tecan M200 reader, in kinetic mode, at 30°C. A negative-control sample with no inhibitor was used, and the background rate (no added FPR) was subtracted from measured rates. IC50s were determined using Prism by fitting the inhibitor concentration (log[I]) and normalized response (V) to the equation V = 100/{10[(logIC50 − log[I])h]}, where h is the Hill coefficient for DprE1. Metabolic stability in vitro. [2] The intrinsic clearance (CLint) of compounds was determined using both mouse and human liver microsomes. Briefly, 100 μg of mouse (CD-1) or human liver microsomes (both from Invitrogen) were mixed in 0.1 M phosphate buffer (pH 7.4) containing 1 μl of compound dissolved in DMSO at 100 μg/ml, in a final volume of 50 μl. In parallel, an NADPH-regenerating system was prepared in 0.1 M phosphate buffer (pH 7.4). The solutions were preincubated at 37°C for 10 min before the intrinsic clearance assessment was initiated by mixing the two solutions (50 μl of each; final compound concentration, 1 μg/ml) at 37°C. After 0, 5, 10, 15, 30, and 60 min, the reactions were terminated by transferring 100 μl of the reaction mixture into 100 μl of acetonitrile and placing the mixture on ice for 30 min, for full protein precipitation. Samples were then centrifuged at 12,000 × g for 10 min, and the supernatant was injected onto a high-performance liquid chromatography (HPLC) column (Dionex) to quantify the amount of parent compound remaining over time. Carbamazepine (1 μg/ml) was used as a control for low intrinsic clearance. MIC/MBC determination. [3] Depending on the setting and requirement, MICs for antituberculosis drugs were determined using the BACTEC TB System, the micro-broth dilution method, the proportion method or the resazurin-reduction method . The MIC was defined as the lowest drug concentration that prevented growth of 99% of the cells and the MBC as the lowest concentration that prevented colony formation on solid medium. Generally the MIC and MBC for BTZ were near-identical. Transcriptomics. [3] M. tuberculosis H37Rv was grown to mid-log phase at 37˚C in Middlebrook 7H9 broth supplemented with 0.05% Tween 80 and albumin- dextrose-catalase (ADC), and exposed to 30 ng/ml BTZ043 for 4h alongside a carrier control. Mycobacterial RNA was extracted using the GTC/Trizol method as developed by Mangan et al., and DNase-treated and purified using RNeasy columns. A M. tuberculosis whole genome microarray, generated by the Bacterial Microarray Group at St. George’s, was utilized to profile the M. tuberculosis response to BTZ. Hybridizations were conducted as previously described, using M. tuberculosis genomic DNA as a common reference. Three biological replicates of BTZ-treated and control cultures were hybridized in duplicate. The hybridized slides were scanned sequentially at 532 nm and 635 nm corresponding to Cy3 and Cy5 excitation maxima using the Affymetrix 428 Array Scanner (MWG). Comparative spot intensities from the images were calculated using Imagene 5.5, and imported into GeneSpring GX 7.2 for further analysis. The array data were normalized to the 50th 2 percentile of all genes detected to be present on the array, and filtered to include only genes flagged to be present on 80% of the arrays. Significantly differentially expressed genes were identified between control and BTZ-treated M. tuberculosis using t-test (p-value <0.05 with Benjamini and Hochberg multiple testing correction) and a fold change of >1.5. Hypergeometric probability (p-value <0.001) was used to identify similar drug exposure signatures derived from previously published datasets. Fully annotated microarray data has been deposited in BµG@Sbase and also ArrayExpress. Proteomics. [3] M. tuberculosis H37Rv was grown in triplicate cultures to OD580 0.3- 0.4, with or without 20 ng/ml of BTZ043, and harvested by centrifugation after 48 h of culturing. The bacterial pellet was washed twice in PBS, resuspended in 10 mM Tris, 250 mM sucrose buffer, pH 7.0, and broken with glass beads using a Mini- Beadbeater. The lysates were sterile filtered and protein concentration determined by the 2-D Quant kit. Sixty µg of each lysate was prepared for 2-D fluorescence difference gel electrophoresis (2-D DIGE) by the 2-D Clean-up kit and dissolved in 30 mM TRIS, 7 M Urea, 2 M Thio-Urea, 4% CHAPS, pH 8.5. Cy2, Cy3 and Cy5 minimal labelling was performed according to the manufacturer's instructions, and 2-D electrophoresis was performed as previously described. Each 2-D gel included a control and a BTZ043-treated sample, as well as a Cy2-labeled internal standard (a pool of all samples in the experiment) to allow correction of inter-gel variation. After electrophoresis, gels were scanned on a Typhoon 9410 gel imager and spot images were analyzed with the Image Master Platinum 2.0 software. The Cy2-labeled standard was used for normalization by the default normalization algorithm, and spots, which displayed more than 2-fold intensity difference, were selected for identification. The 2-D DIGE gels were thereafter silver stained, and the relevant spots excised and identified by MALDI-TOF MS. Comparative analysis of the proteome following BTZ-treatment revealed changes in the levels of several proteins. Consistent increases were seen with the INH-inducible protein IniB (Rv0341) and fumarate hydrolase (Rv1098c), while decreased abundance was observed for two conserved hypothetical proteins (Rv0831c, Rv3716c), and the exported proteins Apa (alanine and proline-rich protein, Rv1860), PepA (serine protease, Rv0125), MPT64 (Rv1980c), Antigen 85B (Rv1886c) and MPT51 (Rv3803c). Most of these changes mirrored those detected by transcriptomics and are hallmarks of cell wall damage. Movie S1 [3] Time-lapse microscopy of BTZ-sensitive M. smegmatis strain (wild-type) exposed to BTZ043. Bacteria were cultivated at 37˚C in a continuous-flow microfluidic device and visualized using the 100X oil immersion objective. Images were acquired at 15 min intervals. Cells were fed standard 7H9 medium for 14.5 h and then exposed to BTZ043 at 0.1 µg/ml (25X MIC) for 74 h. This treatment resulted in lysis of the majority of bacteria. The compound was then washed out and the remaining cells were fed standard 7H9 medium for another 74 h (not shown here). The minority of cells that remained phase dense after BTZ exposure did not recover or resume growth after BTZ washout. When this experiment was performed with the BTZ-resistant M. smegmatis strain, MN84, these effects were not seen. Movie S2 [3] Time-lapse microscopy of BTZ-sensitive M. tuberculosis strain (H37Rv) exposed to BTZ043. Bacteria were cultivated at 37˚C in a continuous-flow microfluidic device and visualized using the 100X oil immersion objective. Images were acquired at 2 h intervals. Cells were fed standard 7H9 medium for 98 h and then exposed to BTZ043 at 0.2 µg/ml for 240 h. The compound was then washed out and the remaining cells were fed standard 7H9 medium for another 265 h. This treatment resulted in lysis of the majority of bacteria. The minority of cells that remained GFP- positive (a) and phase dense (b) after BTZ exposure did not resume growth after BTZ washout. At the end of the experiment the remaining bacteria were stained with propidium iodide (PI), which selectively stains cells with compromised cell wall integrity. The majority of the GFP-positive bacteria were also PI-positive, suggesting that the cell wall permeability barrier had been ruptured and these cells were most likely dead. |
||
| Cell Assay |
BTZ043 displayed similar activity against all clinical isolates of M. tuberculosis that were tested, including extensively drug-resistant and multidrug-resistant strains, indicating that it targets a previously unknown biological function. BTZ043 is bactericidal, reducing viability in vitro by more than 1000-fold in under 72 hours, which is comparable to the INH killing effect.
Preparation of a unicellular Nocardia suspension [1] Because N. brasiliensis grows as filaments, a unicellular suspension was prepared as published previously. N. brasiliensis HUJEG-1 was cultured on Sabouraud agar for 1 week and then sub-cultured in brain heart infusion at 37°C in a shaker at 110 rpm for 72 hrs. The bacterial mass was then separated by centrifugation and washed four times with saline. After grinding in an Evelham-Potter device, the suspension was centrifuged twice at 100 ×g; the supernatant was the unicellular suspension. The bacterial concentration was determined by plating on BHI agar with 5% sheep blood, and the suspension was stored in 20% glycerol at -70°C until use. THP-1 macrophage assays [1] The human monocyte cell line THP-1 was maintained in RPMI 1640 medium supplemented with 10% fetal calf serum (FCS; Gibco-BRL) and 1 mM sodium pyruvate. To transform the cells into macrophages, the cells were sub-cultured four times without sodium pyruvate. The cell density was then determined in a hemocytometer, and the cell suspension was diluted as required in complete RPMI 1640 supplemented with 10% FCS and 6.25 ng/mL phorbol-12-myristate 13-acetate to obtain a density of 4 x 105 cells/mL. A 1 mL aliquot of the cell suspension was seeded into each well of a 24-well microplate, and the cell cultures were washed twice with RPMI 1640 every 48 h for no longer than 4 days. Determination of the intracellular activity of BTZ [1] The technique used has been published previously. Briefly, a 3:1 multiplicity of infection (MOI) was used to determine the effect of antimicrobials on Nocardia intracellular growth. Two hours after infecting the monolayer, the medium was discarded and the monolayer was washed twice with warm PBS, pH 7.4. PBTZ was added at 0.25X, 1X, 4X and 16X the MIC in RPMI 1640 with 10% FCS and incubated for 6 h at 37°C in 5% CO2. We cannot use rifampin as an intracellular active control because N. brasiliensis is a naturally resistant bacteria. Instead, we used DA-7218, an oxazolidinone drug that previously demonstrated good intracellular and in vivo activity against N. brasiliensis. The culture medium was discarded, and 1 mL of cold distilled water was added and incubated for 15 min. To release the intracellular bacteria, the monolayer was disrupted by pipetting up and down several times, and the suspension was collected in 1.5 mL Eppendorf tubes. Nocardia growth was quantified on BHI agar. Decaprenylphosphoryl-β-d-ribose epimerization by M. tuberculosis H37Ra cells. [2] Aliquots of 6 ml of M. tuberculosis H37Ra culture grown to an optical density at 600 nm (OD600) of 1.31 were harvested and washed with buffer A (50 mM MOPS [morpholinepropanesulfonic acid] [pH 7.9], 10 mM MgCl2, 5 mM 2-mercaptoethanol). The cells (∼30 mg) were incubated for 15 min on ice with 50 μl of buffer A, 16 nmol NADH, and 16 μg of PyrBTZ01 or PyrBTZ02 or 2 μg of BTZ043 in 5 μl dimethyl sulfoxide (DMSO), in a final volume of 80 μl. The reactions were started with the addition of 15,000 dpm of 5-phospho-[14C]ribose 1-diphosphate (P[14C]RPP) prepared from [14C]glucose (specific activity, 290 mCi/mmol), as described elsewhere. After 2 h of incubation at 37°C, the reactions were stopped with 1.5 ml CHCl3/CH3OH (2:1) and subjected to a biphasic Folch wash. The organic phase was dried and dissolved in 40 μl of CHCl3/CH3OH/H2O/NH4OH (65:25:3.6:0.5 [vol/vol]); 25% of the sample was separated by thin-layer chromatography on silica gel plates in CHCl3/CH3OH/NH4OH/1 M ammonium acetate/H2O (180:140:9:9:23 [vol/vol]) and visualized by autoradiography (Biomax MR-1 film). The intensity of the bands was quantified using ImageJ software (NIH). Cytotoxicity studies. [2] The cytotoxicity of the compounds was measured as described previously, against two human hepatic cell lines (HepG2 and Huh7), a human lung epithelial cell line (A549), and a human monocytic cell line (THP-1). Briefly, cells were incubated (4,000 cells/well) with serial dilutions of compounds (2-fold dilutions; 100 to 0.1 μg/ml) in a 96-well microplate. Following incubation for 3 days at 37°C, cell viability was determined by adding resazurin for 4 h at 37°C and measuring the fluorescence of the resorufin metabolite (excitation wavelength, 560 nm; emission wavelength, 590 nm) using a Tecan Infinite M200 microplate reader. Data were corrected for background (no-cell control) and expressed as a percentage of the value for untreated cells (cells only). Intracellular activity of BTZ. [3] Raw 264.7 macrophages (1.5 x 108 cells) were infected with H37Rv-GFP at an MOI of 1:1 in 300 ml of RPMI 1640 with 10% heat-inactivated fetal calf serum for 2 h at 37 °C with shaking (100 rpm). After two washes by centrifugation at 1100 rpm for 5 min, the remaining extracellular bacilli from the infected cells suspension were killed by a 1 h amikacin (20 µM) treatment. After a final centrifugation step, cells were dispensed with the Wellmate into 384-well Evotec plates preplated with 10 µl of the respective 3 compound diluted in cell medium. For each compound, a series of 16 two-fold dilutions in quadruplicate was tested. Infected cells were then incubated in the presence of the compound for 5 days at 37 °C, 5% CO2. Then, macrophages were stained with SYTO 60 followed by plate sealing and image acquisition. Confocal images were recorded on an automated fluorescent confocal microscope OperaTM using a 20X-water objective (NA 0.70). Mycobacteria-GFP are detected using a 488-nm laser coupled with a 535/50 nm detection filter and cells labeled with Syto 60 are identified with 635-nm laser coupled with a 690/40 nm detection filter (red channel, Syto 60 excitation). Four independent fields are recorded for each plate well and each image was then processed using dedicated in-house image analysis software to determine five parameters (cell number, cell surface, infected cell number, green objects surface, green surface in infected cells corresponding to bacterial load). Briefly, the algorithm first segments the cells on the red channel using a sequence of processing steps described elsewhere. A similar classification applied on the green channel on pixels above a certain threshold is used to identify green objects. The infected cell number is then defined as those cells having at least a given number of pixels (usually 3) whose intensity in the green channel is above the threshold. The surface of green objects correlates with the number of mycobacteria and its ratio to the total cell number is referred as bacterial load. Typical results of high content screening are shown in fig. S1 where it can be seen that after 5 days, macrophages treated with BTZ043 were abundant and displayed very few GFP-expressing bacilli compared to cells from the negative control (DMSO) or cells treated with the amino-derivative, BTZ045, at the same concentration. In vitro assays of DPA production. [3] For these assays, the preparation of enzymatically active membrane, cell wall-enriched fractions and the radiolabeled substrate (p[14C]Rpp) as well as the reaction mixtures, incubation conditions, and analysis of reaction products were essentially as described previously. In some experiments ~300 µg of protein from cell-free extracts of recombinant E. coli strains expressing Rv3790 and Rv3791 were used to catalyze the reaction. For this purpose the following E. coli strains were used as negative controls or sources of Rv3790 and 4 Rv3791: 1, C41(DE3)/pET28a; 2, C41(DE3)/pET28a-Rv3790-Rv3791; 3, BL21(DE3)/pET28a; 4, BL21(DE3)/pET28a-Rv3791; 5, BL21(DE3)/pET15b; 6, BL21(DE3)/pET15b-Rv3790, 7, BL21(DE3)pLysS/pET32b; 8, BL21(DE3)/pET32b- Rv3790 as indicated in the legend to Figure 3. |
||
| Animal Protocol |
|
||
| ADME/Pharmacokinetics |
Plasma drug concentrations [1]
BTZ043 mouse plasma concentration data have been previously published. At a dose of 100 mg/kg, its plasma concentration reached 4.06 μg/mL (Tmax was 40 min), which is very similar to the plasma concentrations we observed (Figure 2). The Cmax of PBTZ169 was 1.74 μg/mL, and the Tmax was 40 min (Figure 3). Figure 3 also shows the plasma concentration of SXT at a dose of 100 mg/kg, which reached a maximum concentration of 553.88 μg/mL 40 min after administration. t½ was 1.66 h, and AUC was 1507.69 mg/L·h. PyrBTZs and BTZ043 have similar absorption-distribution-metabolism-excretion/toxicity (ADME/T) characteristics. [2] PyrBTZ01 and PyrBTZ02 were tested in parallel with BTZ043 for cytotoxicity (50% toxic dose [TD50]) against four human cell lines (HepG2 hepatocellular carcinoma, Huh7 hepatocellular carcinoma, A549 lung epithelial cells, and THP-1 monocytes) (Table 3). Both compounds showed lower cytotoxicity than BTZ043, with PyrBTZ02 exhibiting the lowest cytotoxicity. BTZ043 had the highest selectivity index (SI) due to its extremely low MIC value, followed by PyrBTZ02 and PyrBTZ01 (Table 3). As previously reported with BTZ043 and PBTZ169, neither PyrBTZ01 nor PyrBTZ02 showed mutagenicity in the SOS chromosome assay. Next, we evaluated the in vitro metabolic stability (intrinsic clearance [CLint]) of PyrBTZ01 and PyrBTZ02 against BTZ043, PBTZ169, and carbamazepine (low CLint control compound) using mouse and human liver microsomes in parallel. In the presence of mouse and human liver microsomes, the CLint values of PyrBTZ01 and PyrBTZ02 were at an intermediate level (Table 4) and similar to those of BTZ043 and PBTZ169, indicating reasonable in vivo compound exposure in mice. To confirm this, we conducted an in vivo pharmacokinetic (PK) study of PyrBTZ01 in BALB/c mice, with a single oral dose of 50 mg/kg. A comparison of the pharmacokinetic (PK) curves of PyrBTZ01 and its analogue BTZ043 at a dose of 25 mg/kg (Figure 4) shows that PyrBTZ01 and BTZ043 have similar half-lives, approximately 100 minutes. The maximum concentration (Cmax) of PyrBTZ01 (approximately 3,500 ng/ml) is higher than that of BTZ043 (1,923 ng/ml), which is likely due to the higher dose of the former rather than higher absorption. |
||
| Toxicity/Toxicokinetics |
Subsequently, we employed a high-content screening method to detect the uptake, intracellular bactericidal activity, and potential cytotoxicity of BTZ compounds in an in vitro model to monitor macrophages infected with GFP-expressing Mycobacterium tuberculosis. Macrophages treated with BTZ043 were protected compared to macrophages treated with the amino derivative BTZ045 or the negative control [dimethyl sulfoxide (DMSO)] (Figure S2). The MIC of BTZ043 was <501 μg/ml) (Figure 1C). In contrast, the MIC of the amino metabolite BTZ045 was >1 μg/ml, consistent with in vitro results (Table S1). As a direct factor related to antibacterial activity, significant macrophage survival was observed when the doses of all compounds were well above the minimum inhibitory concentration (MIC). At the highest tested concentration (10 μg/ml), BTZ043 showed higher cytotoxicity than isoniazid (INH) (Figure 1C), but its selectivity index remained above 100. No particularly adverse effects were found in other in vitro toxicology tests (Table S4). [3]
|
||
| References | |||
| Additional Infomation |
Background: Mycetoma is a neglected chronic teratogenic infectious disease caused by fungi and actinomycetes. In Mexico, Nocardia brasiliensis is the predominant pathogen. Due to the limitations of current drug treatments, there is an urgent need to find alternative therapies. Benzothiazides (BTZs) are a novel class of drug candidates that inhibit decenylphosphoribose epimerase (DprE1), a key enzyme in the biosynthesis of the corynebacterium cell wall. Methods/Main Findings: This study tested the in vitro activity of the next-generation BTZ drug PBTZ169 against 30 Nocardia brasiliensis isolates. The MIC50 and MIC90 values of PBTZ169 were 0.0075 and 0.03 μg/mL, respectively. Since Nocardia is a potentially intracellular bacterium, THP-1 macrophage monolayers were infected with Nocardia brasiliensis HUJEG-1 and then treated with PBTZ169. The results showed a reduction in colony-forming units (CFU) at a concentration 0.25 times the in vitro concentration. In vivo activity was assessed after infection of the right hind leg food pads of female BALB/c mice. Treatment with PBTZ169 was initiated after 6 weeks, and its activity was compared with the first-generation compound BTZ043. Both BTZ compounds were administered twice daily by gavage at a dose of 100 mg/kg, with 100 mg/kg sulfamethoxazole/trimethoprim (SXT) as a positive control. After 22 weeks of treatment, only PBTZ169 and SXT showed statistically significant activity. Conclusion: These results suggest that DprE1 inhibitors may be helpful in treating Nocardia infections and therefore may also be effective against other actinomycete pathogens. We must test the efficacy of these compounds in combination with other antimicrobial agents, such as linezolid, tedeszolid, or trimethoprim-sulfamethoxazole, which have good to excellent in vivo activity, and we also need to test novel DprE1 inhibitors that can achieve higher plasma concentrations. [1] 8-Nitrobenzothiazide compounds (BTZs), such as BTZ043 and PBTZ169, inhibit decapentadiene phosphate-β-D-ribose 2'-oxidase (DprE1) and exhibit nanomolar bactericidal activity against Mycobacterium tuberculosis in vitro. Structure-activity relationship (SAR) studies have shown that the 8-nitro group of the BTZ skeleton is crucial to its mechanism of action, which involves the formation of a hemithyl bond with Cys387 in the active site of DprE1. To date, substitution of the 8-nitro group has resulted in a significant loss of antimycobacterial activity. This article reports the synthesis and characterization of pyrrole-benzothiazinone compounds PyrBTZ01 and PyrBTZ02, two non-nitrobenzothiazinone compounds that retain significant anti-mycobacterial activity with a minimum inhibitory concentration (MIC) of 0.16 μg/ml against Mycobacterium tuberculosis. These compounds exhibited DprE1 inhibitory concentrations (IC50) of less than 8 μM and good in vitro absorption-distribution-metabolism-excretion/toxicity (ADME/T) and in vivo pharmacokinetic characteristics. The most promising compound, PyrBTZ01, did not show efficacy in an acute tuberculosis mouse model, suggesting that the bactericidal effect of BTZ by inhibiting DprE1 requires the combined action of covalent bond formation and compound potency. [2]
New drugs are needed to combat the tuberculosis (TB) pandemic. This article describes the synthesis and characterization of 1,3-benzothiazin-4-one (BTZ), a novel antimycobacterial drug that can kill Mycobacterium tuberculosis in vitro, in vitro, and in mouse models of tuberculosis. Using genetic and biochemical methods, we identified decaisoprene phosphate-β-D-ribose 2'-epimerase as the main target of BTZ. Inhibition of this enzyme activity eliminates the formation of decaisoprene phosphate arabinose, a key precursor in the synthesis of cell wall arabinogalactan, leading to cell lysis and bacterial death. The state-of-the-art compound BTZ043 holds promise for inclusion in combination therapy regimens for drug-sensitive and extensively drug-resistant tuberculosis. [3] |
| Molecular Formula |
C17H16F3N3O5S
|
|---|---|
| Molecular Weight |
431.38
|
| Exact Mass |
431.076
|
| Elemental Analysis |
C, 47.33; H, 3.74; F, 13.21; N, 9.74; O, 18.54; S, 7.43
|
| CAS # |
957217-65-1
|
| Related CAS # |
BTZ043;1161233-85-7
|
| PubChem CID |
49769085
|
| Appearance |
White to light yellow Solid powder
|
| LogP |
3.903
|
| Hydrogen Bond Donor Count |
0
|
| Hydrogen Bond Acceptor Count |
9
|
| Rotatable Bond Count |
1
|
| Heavy Atom Count |
29
|
| Complexity |
720
|
| Defined Atom Stereocenter Count |
0
|
| SMILES |
O=C1C2C=C(C(F)(F)F)C=C(C=2SC(N2CCC3(OC(C)CO3)CC2)=N1)[N+](=O)[O-]
|
| InChi Key |
GTUIRORNXIOHQR-UHFFFAOYSA-N
|
| InChi Code |
InChI=1S/C17H16F3N3O5S/c1-9-8-27-16(28-9)2-4-22(5-3-16)15-21-14(24)11-6-10(17(18,19)20)7-12(23(25)26)13(11)29-15/h6-7,9H,2-5,8H2,1H3
|
| Chemical Name |
2-(2-methyl-1,4-dioxa-8-azaspiro[4.5]decan-8-yl)-8-nitro-6-(trifluoromethyl)-4H-benzo[e][1,3]thiazin-4-one
|
| Synonyms |
BTZ043; BTZ 043; BTZ043 Racemate; 957217-65-1; BTZ043 (Racemate); BTZ038; BTZ043 Racemic; 2-(2-methyl-1,4-dioxa-8-azaspiro[4.5]decan-8-yl)-8-nitro-6-(trifluoromethyl)-4H-benzo[e][1,3]thiazin-4-one; 2-(3-methyl-1,4-dioxa-8-azaspiro[4.5]decan-8-yl)-8-nitro-6-(trifluoromethyl)-1,3-benzothiazin-4-one; BTZ-10526043; BTZ-043; BTZ043 Racemic mixture; BTZ043 Racemate.
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
DMSO : 22~25 mg/mL ( 50.99~57.95 mM )
|
|---|---|
| Solubility (In Vivo) |
Solubility in Formulation 1: 2.5 mg/mL (5.80 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), suspension solution; with sonication.
For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 1.38 mg/mL (3.20 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 13.8 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. View More
Solubility in Formulation 3: 10% DMSO+40% PEG300+5% Tween-80+45% Saline: 2.5 mg/mL (5.80 mM) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.3181 mL | 11.5907 mL | 23.1814 mL | |
| 5 mM | 0.4636 mL | 2.3181 mL | 4.6363 mL | |
| 10 mM | 0.2318 mL | 1.1591 mL | 2.3181 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
|
|---|
|
|
Comparative BTZ efficacy in in vitro, ex vivo, and mouse models.Science.2009 May 8;324(5928):801-4. |
|---|
Inhibition of decaprenylphosphoryl-β-d-ribose epimerization by BTZ.Science.2009 May 8;324(5928):801-4. |
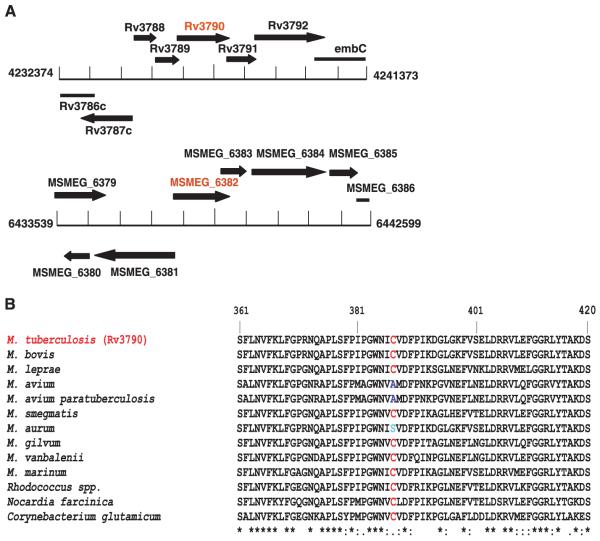 Identification of the BTZ target.Science.2009 May 8;324(5928):801-4. |